Journal of Environmental Studies
Download PDF
Letter to the Editor
*Address for Correspondence: Dejene Sergei V. Jargin, Department of Pathology, People’s Friendship University of Russia, Russia, Tel: +7 495 9516788; E-mail: sjargin@mail.ru
Citation: Jargin SV. Back to Chernobyl: Some Aspects of Cancer Diagnostics. J Environ Stud. 2016;2(1): 8.
Copyright © 2016 Jargin SV. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Environmental Studies | ISSN: 2471-4879| Volume: 2, Issue: 1
Submission: 23 April, 2016 | Accepted: 25 May, 2016 | Published: 30 May, 2016
Reviewed & Approved by: Dr. Jim Clarke, Practice of Civil & Environmental Engineering, Vanderbilt University, USA
Back to Chernobyl: Some Aspects of Cancer Diagnostics
Sergei V. Jargin*
- Department of Pathology, People’s Friendship University of Russia, Russia
*Address for Correspondence: Dejene Sergei V. Jargin, Department of Pathology, People’s Friendship University of Russia, Russia, Tel: +7 495 9516788; E-mail: sjargin@mail.ru
Citation: Jargin SV. Back to Chernobyl: Some Aspects of Cancer Diagnostics. J Environ Stud. 2016;2(1): 8.
Copyright © 2016 Jargin SV. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Environmental Studies | ISSN: 2471-4879| Volume: 2, Issue: 1
Submission: 23 April, 2016 | Accepted: 25 May, 2016 | Published: 30 May, 2016
Reviewed & Approved by: Dr. Jim Clarke, Practice of Civil & Environmental Engineering, Vanderbilt University, USA
Keywords
Ionizing radiation; Chernobyl; Cancer; HistopathologyIntroduction
After the Chernobyl accident massive screening using initially poor equipment, the lack of modern literature and “radiation phobia” contributed to an overdiagnosis of malignancies [1-7]. The “Chernobyl victim syndrome” (i.e. pressure to be registered as a victim) [8] resulted in the registration of patients from noncontaminated areas as having been exposed to radiation. At the time, the exaggeration of Chernobyl’s impact facilitated the financing and creation of numerous doctoral theses. Subsequently, deeper motives for overestimation have emerged - the accident has been exploited for the worldwide strangulation of nuclear energy [9] driven by antinuclear resentments. That said, the attitude of the Green movement has been not without merit: nuclear technologies should have been prevented from spreading to regions where conflicts and terrorism cannot be excluded. Today, there are no alternatives to nuclear energy: non-renewable fossil fuels will become more expensive in the long term, contributing to increased population growth in oilproducing countries and global poverty. Therefore it is time to clarify some mechanisms, unrelated to radiation, that have contributed to the overestimation of medical consequences of the Chernobyl accident.Thyroid Lesions
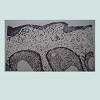
Thyroid cancer in children and adolescents has been the only type of malignancy regarded to have increased significantly due to the Chernobyl accident [10], although early reports of a thyroid cancer increase after the accident were doubted, as radioiodine was thought to have low or no carcinogenicity in humans [11]. The high incidence and short latency were regarded as unusual; the number of thyroid cancers in children and adolescents exposed to radiation was higher than expected [10,12], which led to uncertainty about the accuracy of the diagnoses [13].Another aspect to consider were the differences in diagnostic quality before and after Chernobyl. The introduction of ultrasonography and fine needle aspiration biopsy (FNAB), together with the superficial location of the thyroid, resulted in the detection of numerous thyroid nodules, while suboptimal quality of specimens (Figures 1-6) and insufficient experience with pediatric material contributed to occasional false-positive conclusions about malignancy. The availability of children at schools and kindergartens for mass screening helps to explain the increase in thyroid cancer incidence for this age group. It also accounts for the differences with the Fukushima accident in Japan [11], where screening performed in young people was less dependent on their age. The Fukushima Prefecture program was set up to screen everyone under the age of 19 at the time of the accident. In contrast with Chernobyl, none of the Fukushima thyroid cancer patients were infants at the time of the accident, the majority being adolescents [11].
The proportion of residents who underwent screening after the Fukushima accident during the first screening round decreased year by year: 88% in the 2011 fiscal year, 87% in 2012, and 74% in the 2013 fiscal year; i.e. the time between the accident and tumor detection was around 2 years or less. Accordingly, it was noticed that the incidence of thyroid cancer in the Fukushima area increased more rapidly than expected [14]. This is not surprising - in both Chernobyl and Fukushima, the incidence increased with the screening. The ability of screening to significantly enhance the registered incidence of thyroid cancer is known [9]. Furthermore, lymph node metastases were observed in 40 of 54 thyroid cancer cases after the Fukushima accident, i.e. the tumors were “not at a particularly early stage” [14]. This can be explained by the detection of cases from the “the latent prevalence pool” of undiagnosed cancers [14], which can reasonably be assumed to have been smaller in Japan compared to the former SU due to better coverage of the population by medical check-ups. Note that in areas of poor coverage, some cancers may also remain undiagnosed post mortem. However, the registered childhood thyroid cancer incidence in Japan is low compared to other developed nations [15], suggesting the presence of a sizable pool of undiagnosed thyroid cancers in the population, hence the efficiency of the screening. Given this, the following argument is not convincing: a “clear increase… of thyroid cancer incidence was observed in the second round screening among cases who were screened and cancer free in the first round. This result cannot be explained by the screening effect because most occult thyroid cancer cases would have been harvested in the first round screening” [14]. Note that undiagnosed or occult cancers are not necessarily dormant and could have grown between the screening rounds. In both the Chernobyl and Fukushima areas, differences between the registered thyroid cancer incidence rates in more and less contaminated districts can be explained by differences in screening intensity, participation rate and dose-dependent differences in behavior. People living in more contaminated areas or with knowledge of their higher dose estimates would generally be more motivated to undergo examinations (self-selection bias), and at the same time would be given more attention. The self-selection phenomenon has been noticed in populations exposed to radiation [16,17].
The registered incidence of pediatric thyroid cancer in the former SU before the accident was low compared to other developed countries, which was likely caused by differences in diagnostic quality and coverage of the population by medical checkups. In Belarus, during 1981-1985, the absolute number of thyroid cancers diagnosed in children less than 15 years of age was 3, with 0.3 being the corresponding annual rate per million children under 15 years. For Ukraine, overall there were 25 thyroid cancers diagnosed in children aged 15 years and below, or 0.5 per million. For the northern regions of Ukraine contaminated after the Chernobyl accident these figures were 1.0 and 0.1 [18]. Thyroid cancer is the most frequent malignancy of endocrine glands in children and adolescents, and the above incidence rates are relatively low. Based on the cases diagnosed during 2000-2004, the cancer registry Surveillance, Epidemiology and End Results (SEER) reported an annual age-adjusted incidence rate of 8.5 per 100,000, with approximately 2.1% of the cases being diagnosed in patients under the age of 20, which corresponds to the annual incidence rate in the 0-20 age group of around 1.8 cases per million [19]. Corresponding data from a tumor registry in Germany shows an age-adjusted incidence rate of 2.0 per million for patients aged under 20 years [19]. The United Nations Scientific Committee on the Effects of Atomic Radiation (UNSCEAR) compared the level of enhanced thyroid cancer incidence after the Chernobyl accident not with the pre-accident level, but with the years 1986-1990, when it had already increased up to ~ 5 cases/million. In particular, it was stated that “The background rate of TC among children under the age 10 years is approximately 2 to 4 cases per million per year” [20]. This is much higher than the pre-accident rates discussed above [18].
Considering the low incidence of thyroid cancer prior to the accident, it seems likely that there was a pool of undiagnosed cancers in the population. The percentage of more advanced, histologically less differentiated thyroid cancers was negatively associated with the time between the accident and surgery [21-23], probably due to the gradual exhaustion by the screening of the pool of advanced cases accumulated in the population. Morphologically, thyroid cancers from contaminated territories were reported to be more aggressive than usual [24]. Correlations between radiation doses to the thyroid, tumor invasiveness and a solid-follicular (i.e. a less differentiated) pattern were reported [22,23], but the time factor was not taken into account [22]. Cases with higher doses were probably diagnosed earlier on average, when the pool of neglected cancers was still untapped. As a result, a weak negative correlation between the latency (time from exposure to surgery) and the thyroid dose was found [23]; although “latency” is not an appropriate term if the cause-effect relationship is unproven [25]. The increased incidence of thyroid cancer after the accident was additionally favored by an iodine deficiency in the contaminated territories and an increase of goiter and thyroid nodules [26,27], found by screening, which in turn provided more opportunities for false-positivity.
There were several predisposing factors to a false-positive diagnosis of thyroid carcinoma. During the 1990s, histopathological laboratory equipment was old and primitive [28], with the excessive thickness of histological sections (Figures 1-6) hindering the reliable assessment of histological criteria. Gross dissection of surgical specimens was often made with blunt autopsy or kitchen knives, without washing instruments and cutting boards, and often without access to flowing water, all of which can result in tissue deformation and contamination of the cut surface by cells thus imitating malignancy criteria. This explains the high frequency of tumor cells found in vascular lumina (45%) in post-Chernobyl pediatric thyroid carcinoma [29]. Celloidin embedding was still broadly used, where all nuclei appear somewhat cleared compared to conventional paraffin-embedded specimens, which can be misinterpreted as a sign of papillary carcinoma. The tendency to over-classify the nuclear features of follicular growth-patterned lesions as nuclei of papillary carcinoma-type is known to practitioners, resulting in overdiagnosis of the follicular variant of papillary carcinoma, even in modern laboratories [30]. Pathologists in Russia, who had worked with thyroid tumors from contaminated areas, have pointed out the poor quality of histological specimens interfering with the nuclei assessment [31].
A false-positive diagnosis of thyroid cancer was not excluded after cytological and histological examinations. If a thyroid nodule is found by the screening, a FNAB is performed. Thyroid cytology has a certain percentage of indeterminate results (the so-called gray zone): figures of around 10-20% were reported from modern institutions [32]; but in the former SU the percentage was certainly higher, one of the causes being a shortage of modern literature. Information regarding the sensitivity of FNAB cytology as applied to the pediatric thyroid specimens from contaminated territories was reported: “In a definite or presumptive form, diagnosis of carcinoma was established in 161 from 238 cases”, while papillary carcinoma was diagnosed correctly by cytology in 69.5% of cases and follicular subtype of papillary carcinoma in only 36.5% of all cases [33]. After receiving a cytological report in a presumptive form (“atypical cells” or “suspicion of carcinoma”), a lobectomy or thyroidectomy (discussed below) was performed and the surgical specimen sent for histological examination. After the radical removal of a presumed carcinoma, pathologists sometimes also confirmed malignancy in cases with doubtful histology, thus influencing the statistics. Some histological criteria were hardly known as they were not mentioned by Russianlanguage literature of that time [34,35]. One of the most significant diagnostic terms pertaining to papillary carcinoma - ground-glass or cleared nuclei - was mistranslated as “watch-glass nuclei” and presented by the most widely used handbook of tumor pathology of that time [35] as a feature not only of papillary, but also of follicular carcinoma, which is misleading. Nuclear features, characteristic for papillary carcinoma, are not visible in the illustrations of this handbook [35], which has been reproduced and commented on [36]. In the widely-used Atlas of Tumor Histopathology [37], the following passages on thyroid nodules can be encountered: “In severe dysplasia there appear cell groups with clearly visible atypia. Therefore, 3rd grade dysplasia is considered as an obligate pre-cancer, which histologically is hardly distinguishable from carcinoma in situ”. Accordingly, diagnoses such as “follicular thyroid carcinoma without invasion” or “follicular carcinoma in situ”, suggestive of false-positivity, could be encountered [33]. Note that nuclear atypia is not generally regarded as a malignancy criterion of follicular thyroid nodules/tumors, and the terms “carcinoma in situ” and “dysplasia” are not generally applied to them [30]. Images in handbooks designated as follicular thyroid carcinoma, displaying various degrees of cellular and nuclear atypia [38] without stressing the necessity to search for capsular and vascular invasion (Figure 1), may be conducive to verdiagnosis of thyroid carcinoma, and such cases are known from practice. The tumor capsule should be visible while Hematoxylin-Eosin-Saffron (HES) staining may be convenient for that purpose. Today, with the forthcoming development of molecular markers, the role of cellular characteristics may increase, but until then, images such as Figure 1 in atlases and handbooks may be conducive to false-positivity. Results of verification by expert panels provided further evidence of false-positivity: “As a result of histopathological verification, a diagnosis of thyroid cancer was confirmed in 79.1% of cases (federal level of verification - 354 cases) and 77.9% (international level - 280 cases)” [33]. False-positive cases, not covered by verifications, have remained undisclosed, a situation exacerbated by many archives of histological specimens being in disarray [28]. The retrospective correction of false-positive diagnoses and their prevention in future are suggested due to the risk of possible over-treatment and overmanipulation. The following treatment was recommended for children with supposed radiogenic thyroid cancer: “Radical thyroid surgery including total thyroidectomy combined with neck dissection followed by radioiodine ablation” [39]; “Thyroidectomy and lymph node dissection. Careful and complete removal of the lymph nodes is of great clinical relevance” [40]. Five years after the accident, total thyroidectomy predominated, with hemithyroidectomy utilized only for cancers below 3-5 mm, i.e. microcarcinoma [29].
Some special features of Chernobyl-related pediatric thyroid cancer should be noted. It is known that almost all of them were of papillary type, while solid and follicular (i.e. less differentiated patterns) often predominated [12]. For a pathologist who practiced during Soviet times, the reason is evident. A diagnosis of follicular carcinoma often requires a large number of thin histological sections from the capsular area of a nodule, to search for capsular and vascular invasions. This was not always done for technical reasons and because of insufficient awareness of the minimally invasive follicular carcinoma, absent in Russian-language handbooks of that time [34,35,37]. Therefore, papillary cancer tended to be overdiagnosed, while follicular carcinoma was under-diagnosed. This known tendency [30] must have been increased in conditions of thick slides and insufficient experience with pediatric material. As for the less differentiated histological patterns, their high prevalence was likely caused by the late diagnostics of malignancy.
Urinary Bladder Lesions
Chromosomal rearrangements in the Chernobyl-related thyroid cancer, providing further evidence in favor of the late diagnostics rather than radiogenic nature of the tumors, have previously been discussed [41]. Remarkable figures were reported about thyroid adenoma. The RET/PTC rearrangements were found in 57.1% of the adenomas in patients from non-contaminated areas of Ukraine, but in no cases of thyroid adenomas from France [42]. An explanation can be found in the same article. On re-examination, in 8 of the 14 thyroid adenomas from Ukraine, but in none from France, groups of cells with “limited nuclear features of papillary cancers” were found [42], which sounds unusual in practical pathology and is indicative of diagnostic uncertainty.Diagnostic uncertainty also explains another paradox. In different groups of men (with benign prostatic hyperplasia) and women (with chronic cystitis) from contaminated areas and Kiev, severe urothelial dysplasia and carcinoma in situ (CIS) were found via bladder biopsy in 56-92% of all randomly selected cases [43-47]. The following was observed in patients with benign prostatic hyperplasia studied by bladder biopsy: “Irradiation cystitis with multiple foci of severe urothelial dysplasia/CIS and some invasive transitional cell carcinoma were observed in 96/66, 76/56 and 56/8% of patients in groups I, II and III respectively”. The group III was from non-contaminated areas [46]. In the Handout by the same authors, distributed at the XXIII International Congress of the International Academy of Pathology (IAP) on 15-20 October 2000 in Nagoya, Japan, the following was written: “Histologically the different forms of proliferative cystitis, which were frequently combined and had features of irradiation cystitis with multiple areas of severe dysplasia and carcinoma in situ (CIS), sometimes associated with small transitional-cell carcinoma, occurred in 97% of patients from the radio-contaminated areas of Ukraine”. Such a high prevalence of severe dysplasia and CIS in randomly selected cases is obviously not verisimilar and indicative of false-positivity. Note that over-diagnosis of premalignant and malignant bladder lesions entails over-treatment and over-manipulation, including cystoscopies and biopsies [43-47] which can contribute to the transmission of viral hepatitis [48,49] and other infections. Apparently, “irradiation cystitis” [45,50], reportedly characterized not only by urothelial dysplasia and CIS but also by “reactive epithelial proliferation associated with hemorrhage, fibrin deposits, fibrinoid vascular changes, and multinuclear stromal cells” [50] was caused (at least in part) by repeated cystoscopies, “mapping” biopsies, electrocoagulation etc. Accordingly, it can be reasonably assumed that some of the biomarkers, especially those associated with inflammation and cell proliferation (TGF-β1, mitogen-activated protein kinases, growth factors, etc.), as well as the “marked activation of angiogenesis” [45], partly reflected iatrogenic inflammation and repair.
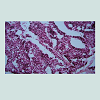
In studies of bladder lesions [43-47], described histological differences between the exposed and unexposed cohorts may have been related to the quality of specimens and their assessment. In this regard, the images from [45] should be noted (Figures 2 and 3). Some images from [45] and [47] published 9 years apart, are identical. The same is true for earlier articles involving the same scientists [51,52]. Apparently, over-diagnosis of dysplastic and neoplastic bladder lesions had also occurred previously - both articles [51,52] used the same image of bladder leukoplakia with invasion according to the caption but invasive growth is not clearly recognizable (Figure 4).
Figure 3: From the caption [45]: dysplasia (A-D) and small papillary urothelial carcinoma (E-G). Comment: mild to moderate atypia might be present in A-D; butno severe dysplasia is recognizable. Figure E: nuclei are poorly stained probably due to an electrocoagulation artefect. All the slides are obviously too thick for reliable diagnostics.
Typical radiation-induced changes of squamous and transitional epithelium, known from biopsies after therapeutic irradiation, are absent in these and other images, which was commented in the article: “Classic descriptions of acute and chronic radiation effects on the urinary bladder do not coincide with the pathogenesis of human urinary bladder injury after long-term, low-dose exposure to ionizing radiation” [45]. Histological images of the bladder mucosa and thyroid, potentially conductive to the over-diagnosis of malignancy, can be seen in widely-used editions [34,35] on tumor histopathology (Figures 5 and 6).
The mean activity concentration of cesium-137 in urine in the most exposed group of patients was 6.47 Bq/liter [44,45]. For comparison, the guidance level for cesium-137 in drinking water is 10 Bq/liter [53], but it would be higher in urine due to renal concentration. Possible radiation doses resulting from such concentration were discussed previously [5]: the doses would be too low to cause any increase in bladder malignancy or the “radiation induced chronic proliferative atypical cystitis,” reportedly characterized by multiple areas of severe dysplasia and CIS [45].
Discussing urological concerns, one more study [54] should be mentioned: in 75.6% of testicles randomly sampled post mortem (forensic cases, residents of Kaluga province in Russia partly belonging to the contaminated territories [7,10] in comparison with controls from non-contaminated areas) was found paucity or absence of germ cells, affecting more than 10% of spermatic tubules, which was explained by radiation exposure. Considering that the individual radiation doses in Kaluga area remained within the limits of natural radiation background (additional dose for the period 1986-95 was about 4 mSv [10], the global average annual dose from the natural radiation background - 2.4 mSv), the cause-effect relationship with radiation is improbable. This is similar to many other publications on Chernobyl consequences, where various structural derangements, sometimes compatible with the norm (Figure 7), were a priori considered as radiogenic, overviewed in [5,55,56].
Figure 7: A microphotograph of testicular tissue. Hypospermatogenesisaccording to the caption [54]. The histological picture is compatible with the norm.
Renal Tumors
Poorly substantiated information was also published on other alleged radiation-related conditions; the statement that “during the 25-year period subsequent to the Chernobyl accident, the morbidity of malignant renal tumors in Ukraine has increased from 4.7 to 10.7 per 100,000 of the total population” [57] was supported by a reference to a report by Ukraine’s Ministry of Health. Despite this however, the incidence increase of renal cell carcinoma due to the Chernobyl fallout has not been scientifically proven, while some of the increase may have been caused by improved diagnostics and coverage of the population by medical checkups [58]. The statement -“recent studies of our group have shown that increases in morbidity, aggressiveness, and proliferative activity of renal cell carcinomas, especially clear-cell carcinoma, in Ukrainian patients that have continuously inhabited the radio-contaminated areas, might be explained by specific molecular events, influenced by chronic persistent low-dose ionizing radiation exposure” [57] was supported by self-references [59,60]. In these, it was claimed that “The strong significant differences between the Ukrainian and Spanish groups were found in tumoral nuclear grade” [59] and, “Our data showed in the majority of Ukrainian patients a radiation sclerosing proliferative atypical nephropathy in association with an increase in the incidences of tubular epithelial nuclear atypia and carcinoma in situ” [60]. It was reported that in 73% of renal cancer patients from contaminated territories and 72% of those from non-contaminated areas of Ukraine, the tumor displayed a high level of microvessel density - the average level in the combined Ukrainian groups was 1.65 times higher than in the Spanish control group [57]. Radiation exposure was connected with the elevation of microvessel density and a higher histological grade, sarcomatoid transformation and intratumoral necrosis [57] i.e. histological signs of de-differentiation. An association of microvessel density with the cancer grade is acknowledged [61] but the difference in the histological grade can be explained by the averagely earlier detection of malignancies in Spain when compared to Ukraine. Accordingly, the higher microvessel density in renal cancers from Ukraine, as well as the higher grade of Chernobyl-related cancers in general [24], were caused by detection of neglected cases after the accident. Morphologic and molecular-genetic differences between renal cell carcinoma from Ukraine and Spain [57,59,60] were caused by the earlier detection of malignancies in Spain; as discussed in [58,62].Considering the above, the results of some studies are interpretable but would benefit from re-evaluation. For example, the following has been reported: “These findings do not allow us to consider the immunohistochemical expression of ubiquitylation and sumoylation as valuable markers for discriminating the effects of long-term, lowdose ionizing radiation exposure in conventional renal cell carcinoma carcinogenesis” [63]. Considering that cancers from Ukraine were generally more advanced than the controls from Spain, the results of this study suggest that ubiquitylation and sumoylation are not associated with the progression of renal cell carcinoma.
Conclusion
The above and previously published [1-6] arguments question the generally accepted cause-effect relationship between ionizing radiation and cancer incidence increase after the Chernobyl accident. With regard to Chernobyl-related pediatric thyroid cancer, this causeeffect relationship cannot be excluded, but the registered increase in incidence can be largely attributed to factors other than radiation. Accordingly, some studies searching for markers of radiogenic cancer, e.g. [64], were probably based on the unproven premise that all or a majority of malignancies in the contaminated areas had been caused or influenced by ionizing radiation. Another important point in this discussion is that many tumors detected during the first decade after the accident, whether due to improved screening and diagnostics, or in patients being brought from non-contaminated areas and falsely registered as Chernobyl victims, were already advanced cancers: “The tumors were randomly selected (successive cases) from the laboratories of Kiev and Valencia... [The cancers were] clearly more aggressive in the Ukrainian population in comparison with the Valencian cases” [65]. This phenomenon can however be explained due to the (on average) earlier diagnostics of malignancies in Western Europe. In conclusion, the exaggeration of Chernobyl’s consequences could lead to the overestimation of the carcinogenicity of certain radionuclides. This result may potentially be detrimental to research, medical practice and economic advancements.Acknowledgements
The author is sincerely grateful to Professor Jim Clarke and Kaatrin Abbott for advice leading to a considerable improvement of the manuscript.References
- Jargin SV (2014) Chernobyl-related cancer and precancerous lesions: Incidence increase vs. late diagnostics. Dose Response 12: 404-414.
- Jargin SV (2015) Solid cancer increase among Chernobyl liquidators: alternative explanation. Radiat Environ Biophys 54: 373-375.
- Jargin SV (2012) Debate on the Chernobyl disaster: on the causes of Chernobyl overestimation. Int J Health Serv 42: 29-34.
- Jargin SV (2016) Biological effectiveness of ionizing radiation: acute vs. protracted exposures. J Environ Stud 2: 5.
- Jargin SV (2009) Overestimation of Chernobyl consequences: biophysical aspects. Radiat Environ Biophys 48: 341-344.
- Jargin SV, Kaloshin AK (2015) Back to the Mechanisms of Cancer Incidence Increase after Chernobyl. Int J Cancer Res Mol Mech 1.
- Mould RF (2000) Chernobyl record. The definite history of the Chernobyl catastrophe. Institute of Physics Publishing Bristol and Philadelphia. CRC Press.
- Bay IA, Oughton DH (2005) Social and economic effects. In: Smith JT, Beresford NA (Eds). Chernobyl-catastrophe and consequences. Springer: Chichester, UK, pp. 239-266.
- Jaworowski Z (2010) Observations on the Chernobyl disaster and LNT. Dose Response 8: 148-171.
- United Nations Scientific Committee on the Effects of Atomic Radiation (2000) UNSCEAR 2000 Report to the General Assembly (Vol 2). Sources and effects of ionizing radiation. Annex J Exposures and effects of the Chernobyl accident. United Nations, New York.
- Williams D (2015) Thyroid growth and cancer. Eur Thyroid J 4: 164-173.
- IARC (2001) Thyroid cancer in young people. Ionizing radiation, Part 2. In: IARC monographies on the evaluation of carcinogenic risks to humans 78: 233-236.
- Lushnikov EF, Tsyb AF, Yamashita S (2006) Thyroid cancer in Russia after the Chernobyl. Meditsina, Moscow, pp. 36-59.
- Tsuda T, Tokinobu A, Yamamoto E, Suzuki E (2016) Thyroid cancer detection by ultrasound among residents ages 18 years and younger in Fukushima, Japan: 2011 to 2014. Epidemiology 27: 316-322.
- International Agency for Research on Cancer (1999) International incidence of childhood cancer. IARC Scientific Publication 144.
- McGeoghegan D, Binks K, Gillies M, Jones S, Whaley S (2008) The non-cancer mortality experience of male workers at British Nuclear Fuels plc, 1946-2005. Int J Epidemiol 37: 506-518.
- Zablotska LB, Bazyka D, Lubin JH, Gudzenko N, Little MP, et al. (2013) Radiation and the risk of chronic lymphocytic and other leukemias among chornobyl cleanup workers. Environ Health Perspect 121: 59-65.
- Stsjazhko VA, Tsyb AF, Tronko ND, Souchkevitch G, Baverstock KF (1995) Childhood thyroid cancer since accident at Chernobyl. BMJ 310: 801.
- Luster M, Lassmann M, Freudenberg LS, Reiners C (2007) Thyroid cancer in childhood: management strategy, including dosimetry and long-term results. Hormones (Athens) 6: 269-278.
- UNSCEAR (2008) Report to the General Assembly. Effects of ionizing radiation. Annex D. Health effects due to radiation from the Chernobyl accident, Vol 2, United Nations, New York.
- Williams ED, Abrosimov A, Bogdanova T, Demidchik EP, Ito M, et al. (2004) Thyroid carcinoma after Chernobyl latent period, morphology and aggressiveness. Br J Cancer 90: 2219-2224.
- Bogdanova TI, Zurnadzhy LY, Nikiforov YE, Leeman-Neill RJ, Tronko MD, et al. (2015) Histopathological features of papillary thyroid carcinomas detected during four screening examinations of a Ukrainian-American cohort. Br J Cancer 113: 1556-1564.
- Zablotska LB, Nadyrov EA, Rozhko AV, Gong Z, Polyanskaya ON, et al. (2015) Analysis of thyroid malignant pathologic findings identified during 3 rounds of screening (1997-2008) of a cohort of children and adolescents from Belarus exposed to radioiodines after the Chernobyl accident. Cancer 121: 457-466.
- 24. Yablokov AV (2009) Oncological diseases after the Chernobyl catastrophe. Ann N Y Acad Sci 1181: 161-191.
- Jargin SV (2009) Overestimation of Chernobyl consequences: calculation of a latent period for tumors with unproven radiation etiology. Radiat Environ Biophys 48: 433-434.
- Hatch M, Polyanskaya O, McConnell R, Gong Z, Drozdovitch V, et al. (2011) Urinary Iodine and Goiter Prevalence in Belarus: experience of the Belarus-American cohort study of thyroid cancer and other thyroid diseases following the Chornobyl nuclear accident. Thyroid 21: 429-437.
- Kholodova EA, Fedorova LP (1992) Prevalence of endemic goiter in Belarus. Probl Endokrinol (Mosk) 38: 30-31.
- Jargin SV (2010) The practice of pathology in Russia: On the eve of modernization. Basic Appl Pathol 3: 70-73.
- Demidchik EP, Tsyb AF, Lushnikov EF (1996) Thyroid carcinoma in children. Consequences of Chernobyl accident (in Russian). Meditsina, Moscow.
- Sobrinho-Simões M, Eloy C, Magalhães J, Lobo C, Amaro T (2011) Follicular thyroid carcinoma. Mod Pathol 24 Suppl: S10-S18.
- Abrosimov AIu, Lushnikov EF, Frank GA (2001) Radiogenic (Chernobyl) thyroid cancer. Arkh Patol 63: 3-9.
- Chow LS, Gharib H, Goellner JR, van Heerden JA (2001) Nondiagnostic thyroid fine-needle aspiration cytology: management dilemmas. Thyroid 11: 1147-1151.
- Abrosimov AIu (2004) Thyroid carcinoma in children and adolescents of Russian Federation after the Chernobyl accident. Doctoral dissertation. Obninsk.
- Bomash NIu (1981) Morphological diagnostics of thyroid diseases, Meditsina, Moscow.
- Kraievski NA, Smolyannikov AV, Sarkisov DS (1993) Patho-morphological diagnostics of human tumors. Meditsina, Moscow.
- Jargin SV (2011) Pathology in the former Soviet Union: scientific misconduct and related phenomena. Dermatol Pract Concept 1: 75-81.
- Paltsev MA, Anichkov NM (2005) Atlas of human tumor pathology. Moscow: Meditsina.
- Shkurupii VA, Poloz TL (2009) Cytomorphology of thyroid follicular tumors. Russian Academy of Medical Sciences: Novosibirsk.
- Demidchik YE, Saenko VA, Yamashita S (2007) Childhood thyroid cancer in Belarus, Russia, and Ukraine after Chernobyl and at present. Arq Bras Endocrinol Metabol 51: 748-762.
- Reiners C, Demidchik YE, Drozd VM, Biko J (2008) Thyroid cancer in infants and adolescents after Chernobyl. Minerva Endocrinol 33: 381-395.
- Jargin SV (2015) On the RET/PTC3 rearrangements in Chernobyl-related thyroid cancer vs. late detection. Int J Cancer Res Mol Mech 1.
- Di Cristofaro J, Vasko V, Savchenko V, Cherenko S, Larin A, et al. (2005) ret/PTC1 and ret/PTC3 in thyroid tumors from Chernobyl liquidators: comparison with sporadic tumors from Ukrainian and French patients. Endocr Relat Cancer 12: 173-183.
- Romanenko A, Morimura K, Wei M, Zaparin W, Vozianov A, et al. (2002) DNA damage repair in bladder urothelium after the Chernobyl accident in Ukraine. J Urol 168: 973-977.
- Romanenko AM, Kinoshita A, Wanibuchi H, Wei M, Zaparin WK, et al. (2006) Involvement of ubiquitination and sumoylation in bladder lesions induced by persistent long-term low dose ionizing radiation in humans. J Urol 175: 739-743.
- Romanenko A, Kakehashi A, Morimura K, Wanibuchi H, Wei M, et al. (2009) Urinary bladder carcinogenesis induced by chronic exposure to persistent low-dose ionizing radiation after Chernobyl accident. Carcinogenesis 30: 1821-1831.
- Romanenko A, Fukushima S (2000) Prediction of urinary bladder cancer induction in Ukraine after the Chernobyl accident. XXIII International Congress of the International Academy of Pathology and 14th World Congress of Academic and Environmental Pathology. 15-20 October 2000, Nagoya, Japan. Pathol Int 50 (Suppl): A70.
- Romanenko A, Morimura K, Wanibuchi H, Salim EI, Kinoshita A, et al. (2000) Increased oxidative stress with gene alteration in urinary bladder urothelium after the Chernobyl accident. Int J Cancer 86: 790-798.
- Saludes V, Esteve M, Casas I, Ausina V, Martró E (2013) Hepatitis C virus transmission during colonoscopy evidenced by phylogenetic analysis. J Clin Virol 57: 263-266.
- Vanhems P, Voirin N, Trépo C, Trabaud MA, Yzèbe D, et al. (2003) The risk of hospital-acquired GB virus C infection: a pilot case-control study. J Hosp Infect 53: 72-75.
- Romanenko A, Vozianov A, Morimura K, Fukushima S (2001) Correspondence re: W. Paile's letter to the editor. Cancer Res., 60: 1146, 2000. Cancer Res 61: 6964-6965.
- Romanenko AM (1982) Chronic cystitis in the aspect of its relationship with precancerous conditions. Arkh Patol 44: 52-58.
- Romanenko AM, Klimenko IA, Iurakh GIu (1985) Leukoplakia of the bladder. Arkh Patol 47: 52-58.
- World Health Organization (2006) Guidelines for drinking-water quality: incorporating first addendum. Vol. 1, Recommendations, (3rdedn). Radiation aspects. Electronic version for the Web, pp. 197-209.
- Lysenko AI, Kirpatovskii ID, Pisarenko SS (2000) Morphological changes in male sexual glands in Kaluga regions contaminated with radionuclides. Arkh Patol 62: 27-31.
- Jargin SV (2011) Thyroid cancer after Chernobyl: obfuscated truth. Dose Response 9: 471-476.
- Jargin SV (2010) Overestimation of Chernobyl consequences: poorly substantiated information published. Radiat Environ Biophys 49: 743-745.
- Romanenko AM, Ruiz-Saurí A, Morell-Quadreny L, Valencia G, Vozianov AF, et al. (2012) Microvessel density is high in clear-cell renal cell carcinomas of Ukrainian patients exposed to chronic persistent low-dose ionizing radiation after the Chernobyl accident. Virchows Arch 460: 611-619.
- Jargin SV (2015) Renal cell carcinoma after Chernobyl: on the role of radiation vs. late detection. Pathol Oncol Res 21: 845-846.
- Romanenko A, Morell-Quadreny L, Nepomnyaschy V, Vozianov A, Llombart-Bosch A (2000) Pathology and proliferative activity of renal-cell carcinomas (RCCS) and renal oncocytomas in patients with different radiation exposure after the Chernobyl accident in Ukraine. Int J Cancer 87: 880-883.
- Romanenko A, Morell-Quadreny L, Nepomnyaschy V, Vozianov A, Llombart-Bosch A (2001) Radiation sclerosing proliferative atypical nephropathy of peritumoral tissue of renal-cell carcinomas after the Chernobyl accident in Ukraine. Virchows Arch 438: 146-153.
- Kavantzas N, Paraskevakou H, Tseleni-Balafouta S, Aroni K, Athanassiades P, et al. (2007) Association between microvessel density and histologic grade in renal cell carcinomas. Pathol Oncol Res 13: 145-148.
- Jargin SV (2007) Over-estimation of radiation-induced malignancy after the Chernobyl accident. Virchows Arch 451: 105-106.
- Morell-Quadreny L, Romanenko A, Lopez-Guerrero JA, Calabuig S, Vozianov A, et al. (2011) Alterations of ubiquitylation and sumoylation in conventional renal cell carcinomas after the Chernobyl accident: a comparison with Spanish cases. Virchows Arch 459: 307-313.
- Akulevich NM, Saenko VA, Rogounovitch TI, Drozd VM, Lushnikov EF, et al. (2009) Polymorphisms of DNA damage response genes in radiation-related and sporadic papillary thyroid carcinoma. Endocr Relat Cancer 16: 491-503.
- Romanenko A, Morell-Quadreny L, Ramos D, Nepomnyaschiy V, Vozianov A, et al. (2007) Author reply to: over-estimation of radiation-induced malignancy after the chernobyl accident. Virchows Arch 451: 107-108.