Journal of Pharmaceutics & Pharmacology
Download PDF
Review Article
*Address for Correspondence: Annesha Lovett, PharmD, MS, PhD, College of Pharmacy & Health Sciences, 3001 Mercer University Drive, Office #138 Atlanta, GA 30341, Tel: 678-547-6134; Fax: 678-547-6384; E-mail: lovett_aw@mercer.edu
Citation: Lovett A, Rakestraw K. A Review of Community Pharmacy-Based Pharmacologic Interventions and Methods for Smoking Cessation. J Pharmaceu Pharmacol. 2013;1(1): 8.
Copyright © 2013 Lovett A, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Pharmaceutics & Pharmacology | ISSN: 2327-204X | Volume: 1, Issue: 1
A Review of Community Pharmacy-Based Pharmacologic Interventions and Methods for Smoking Cessation
Annesha Lovett and Katherine Rakestraw*
- College of Pharmacy & Health Sciences, 3001 Mercer University Drive, Office #138 Atlanta, USA
*Address for Correspondence: Annesha Lovett, PharmD, MS, PhD, College of Pharmacy & Health Sciences, 3001 Mercer University Drive, Office #138 Atlanta, GA 30341, Tel: 678-547-6134; Fax: 678-547-6384; E-mail: lovett_aw@mercer.edu
Citation: Lovett A, Rakestraw K. A Review of Community Pharmacy-Based Pharmacologic Interventions and Methods for Smoking Cessation. J Pharmaceu Pharmacol. 2013;1(1): 8.
Copyright © 2013 Lovett A, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Pharmaceutics & Pharmacology | ISSN: 2327-204X | Volume: 1, Issue: 1
Abstract
Background: The aim of this study was to provide an overview of the published peer-reviewed literature related to community pharmacy-based smoking cessation counseling efforts in the United States and Canada.Methods: Electronic databases, Embase, PubMed and Medline, were searched for articles from January 2002 to January 2012. Keywords used were smoking cessation, pharmacist, pharmacologic, pharmacy, and multidisciplinary. Studies were excluded if they were conducted outside of the United States and Canada.
Results: Twenty-six articles were included in this review with subtopics pharmacist and patient perception of pharmacy-based counseling, pharmacologic interventions, and methods for pharmacist led smoking cessation counseling. Literature review suggests both patients and pharmacists have positive views on smoking cessation counseling by a pharmacist. Studies show that counseling related to pharmacologic interventions is preferred. Specifically, patients prefer a non-confrontational approach by pharmacists. Although the 2008 Clinical Practice Guidelines, Treating Tobacco Use and Dependence, recommend an intensive intervention approach due to a strong dose-response relationship between the session length and successful treatment outcomes, pharmacists are unlikely to use an intensive intervention. Pharmacists should perform brief counseling sessions by assessing a patient’s willingness to quit and then motivating, educating, and referring them to an available resource. These brief sessions should be done in person and performed at each visit.
Conclusions: Pharmacists are encouraged to develop or adopt a system of tracking codes for smoking cessation counseling as efforts towards reimbursement increase in the future. Evidence suggests that cost reduction and improved health outcomes can occur when smoking cessation counseling is provided in the community pharmacy setting. Future research should examine reimbursement for pharmacistprovided counseling.
Keywords: Smoking cessation; Pharmacist counseling; Community pharmacy
Introduction
According to the Surgeon General cigarette smoking is the leading cause of death in the United States accounting for one of every five deaths each year [1]. Smoking causes more deaths than HIV, illegal drug use, alcohol use, motor vehicle injuries, suicides, and murders combined. Smoking results in a harmful impact on nearly every organ of the body [2]. When comparing smokers to nonsmokers there is an increased risk of coronary artery disease and stroke by 2-4 times. Furthermore, men and women who smoke are 23 and 13 times more likely to develop cancer, respectively [1].While the prevalence of Americans who smoke decreased from 42.4% in 1965 to 24.7% in 1997, the rate of tobacco use among both men and women has remained constant since 1990 [3]. According to the 2008 Clinical Practice Guidelines for Treating Tobacco Use andDependence, approximately 19.8% of Americans currently smoke cigarettes. The guidelines recommend a systematic effort by all health care providers (HCPs) to implement cessation counseling as part of their routine practice [4].
While the guidelines are intended for use by all clinicians, including pharmacists, a clinician with a Doctor of Pharmacy degree or a pharmacist with a registered license was not cited in the panel of HCPs used for the 2008 updates. Liaisons and staff persons included those with a master degree in public health, the science of nursing, education, and members certified as health education specialists. Consequently, those who developed the guidelines may have failed to recognize that the pharmacist has the ability to play a key role in counseling for smoking cessation. The U.S. Department of Health and Human Services 2000 report entitled, Treating Tobacco Use and Dependence, states both cognitive behavioral therapy and pharmacotherapy are needed to increase the likelihood of patients successfully quitting [5]. Because smoking cessation related medications are available primarily through a pharmacy, and nicotine replacement therapy (NRT) products are available over the counter, pharmacists have the unique opportunity of being a specialized resource for patients who are either thinking about or attempting to quit smoking.
The Healthy People 2020 initiative has set a goal of reducing the number of American’s that smoke to 12% and increasing smoking cessation attempts from 48.3% to 80% [6]. The initiative aims to increase smoking cessation attempts and successes using evidencebased strategies. Additional goals have been set to increase smoking cessation counseling in office-based and hospital ambulatory care settings, dental care settings, and substance abuse care settings [6].
However, like the Clinical Practice Guidelines, the Healthy People initiative fails to set goals specifically for a pharmacy setting and focuses more on ambulatory and dental care settings. While there are many studies suggesting the importance of the role of physicians in smoking cessation, few studies are available pertaining to pharmacists or multidisciplinary efforts. The objective of this study was to provide an overview of the literature related to community pharmacy-based smoking cessation efforts in the United States and Canada.
Methods
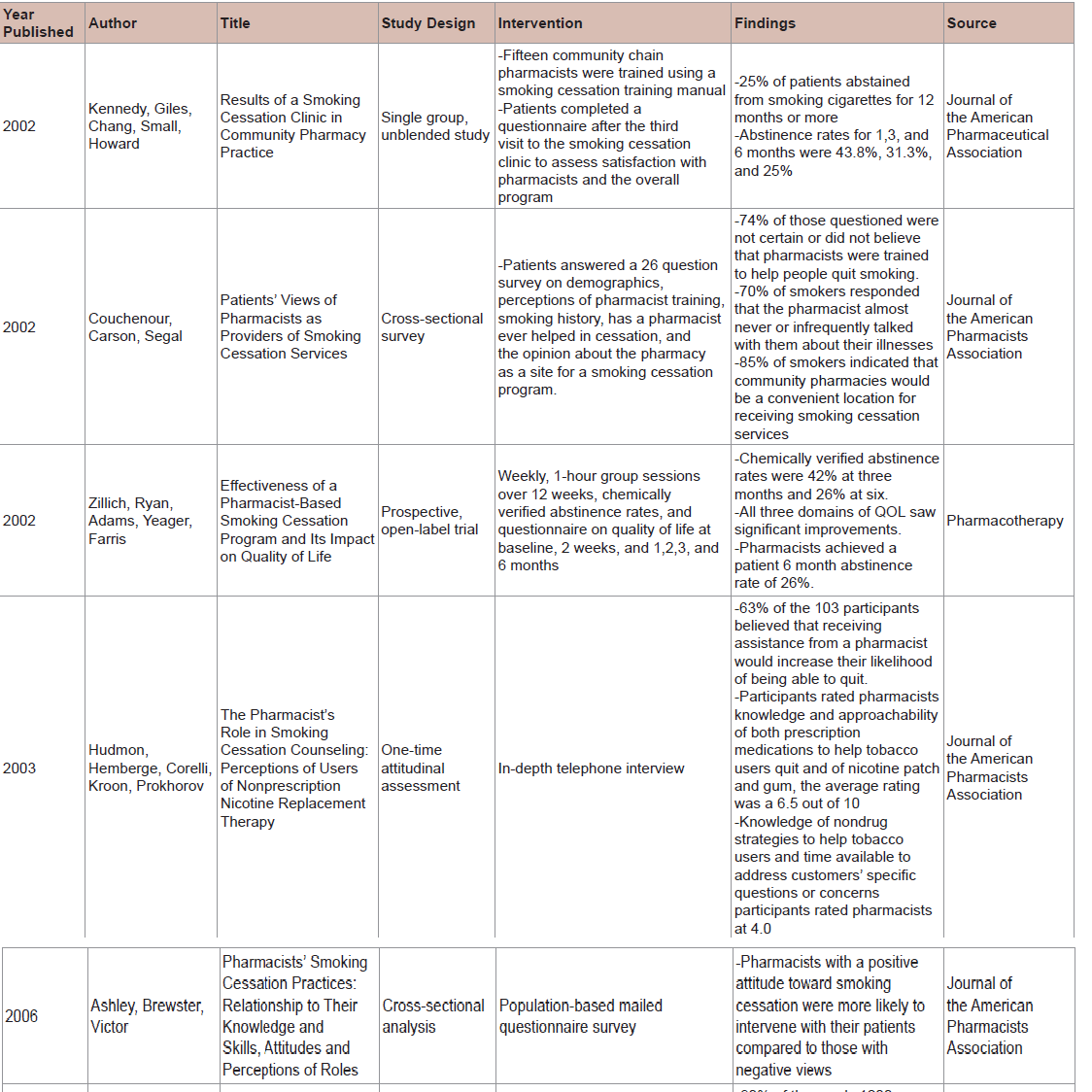
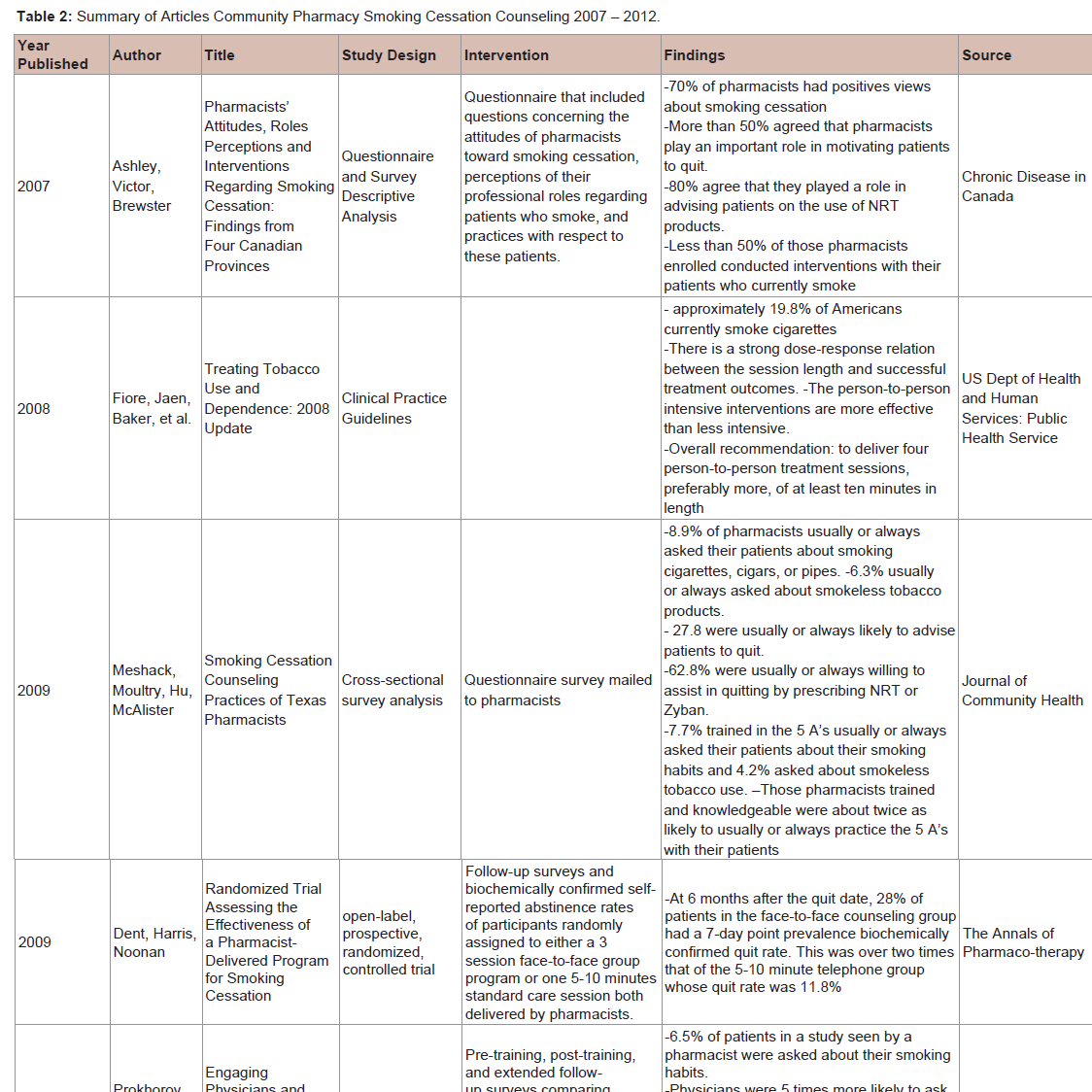
Electronic databases, Embase, PubMed and Medline, were searched for articles from January 2002 to January 2012. This timeframe was selected as prior to 2002 there were existing studies that provided a review of smoking cessation efforts. It should be noted that those studies focused on roles other than the pharmacist’s role (such as the role of physicians). Key words used in the search strategy were ‘smoking cessation’, and ‘pharmacist’, or ‘pharmacy’, or ‘pharmacologic’, or ‘multidisciplinary’. Studies were excluded if they were conducted outside of the United States and Canada. The bibliographies of retrieved references were scanned for relevant publications.The quality of articles was assessed by one author and then checked by a second author. Pooling of studies was not possible due to the heterogeneity of participants, outcomes, and interventions across studies. The following information was noted in a structured summary table: year published, author, title, study design, intervention, findings, and source (Tables 1 and 2). Additionally, the following subtopics were utilized to summarize results: patient and pharmacist perceptions on smoking cessation counseling, pharmacologic interventions, and methods for pharmacist led smoking cessation counseling.
Results
Twenty-six articles were included in this review, 8 on pharmacist and patient perception of pharmacy-based counseling, 7 on pharmacologic interventions, and 11 on methods for pharmacist led smoking cessation counseling.Patient and pharmacist perceptions on smoking cessation counseling
In a study published in 2002, a survey of 73 patients found that 74% of those questioned were not certain or did not believe that pharmacists were trained to help people quit smoking. Seventy percent of smokers who were questioned responded that the pharmacist almost never or infrequently talked with them about their illnesses. Yet, respondents who indicated that their pharmacist almost always or frequently talked with them about their medications were most likely to either strongly agree or agree that pharmacists were trained to help people quit smoking. Findings suggested that pharmacists who engaged with their patients were viewed as more helpful. It was also suggested that patients needed to become more aware of the community pharmacist as a resource for smoking cessation assistance as 85% of smokers indicated that community pharmacies would be a convenient location for receiving smoking cessation services [7].
One year later, a study was published on the public’s perception of the pharmacist’s role in smoking cessation. While this study did not look explicitly at whether or not a pharmacist was qualified to counsel on smoking cessation, 63% of the 103 participants believed that receiving assistance from a pharmacist would increase their likelihood of being able to quit. When participants were asked to rate pharmacist’s knowledge and approachability of both prescription medications to help tobacco users quit and of the nicotine patch and gum, the average rating was a 6.5 out of 10 (10 being excellent and 1 being poor). However, pharmacist knowledge of nondrug strategies to help tobacco users and time available to address customers’ specific questions or concerns was rated as 4.0 out of 10 [8].
Furthermore, participants were asked to rate the appropriateness of pharmacists’ involvement in specific phases of tobacco cessation. With 10 being extremely appropriate and 1 being not at all appropriate, educating customers about the use of nicotine patches and gum was deemed most appropriate with a score of 8.7 out of 10 while helping smokers set a quit date was lowest at 5.8 out of 10. Participants rated pharmacist involvement in offering specific product recommendations for helping people quit smoking at 7.8 out of 10, offering appointments to talk by phone or in person to check on patients progress at 7.0 out of 10, and asking smokers to keep them informed of their progress towards quitting at 6.8 out of 10. Overall, pharmacists’ involvement in tobacco cessation was averaged to be 6.9 out of 10 [8].
Lastly, the study asked participants how they perceived the usefulness of discussing specific smoking cessation-related topics with their pharmacist by answering with either a 0 (not at all useful) or 4 (extremely useful). The following are the percentages of patients which found pharmacists either very or extremely useful in various categories: 92% in side effects of smoking cessation medications, 84.5% in withdrawal symptoms, 80% in different medications and strategies for quitting, and 78.6% on the effects of continued tobacco use on health. Although the majority (>80%) of patients ranked pharmacists as either very or extremely useful in discussing which medications to use and their side effects, only 77.2% of participants found pharmacists to be very or extremely useful in discussing the importance of compliance with the nicotine patch or gum regimens [8].
In 2010, Patwardhan and colleagues conducted 24 semistructured telephone interviews with tobacco users, with an aim to generate hypotheses and theoretical explanations of perceptions related to smoking cessation. The interview consisted of open-ended and neutrally worded questions to avoid eliciting desirable responses. Eight themes were found, two of which involved the perception of the pharmacist. Nine of the 24 interviewees stated that ask, advise, refer (AAR) counseling was appropriate if provided by a community pharmacist. However, it was suggested that interviewees responded in this way due to concerns about tobacco smoking interacting with their medications. Ten of the 24 interviewees commented on the smoker’s sensitivity toward the topic of their tobacco use. Thus, it was concluded that a non-confrontational approach was best. This was the second most commented theme with AAR counseling (the first was appropriateness). It is important to note that 4 interviewees agreed that AAR counseling would be perceived as less appropriate if the smoker was not ready to quit at the time of counseling. However, overall results of this study suggest that tobacco users would be receptive to AAR counseling at their community pharmacies as long as it was conducted in a professional and respectful manner [9].
Studies reveal that pharmacists have similar views to patients in regard to their role in smoking cessation counseling. When examining pharmacists across Canada, a study found that more than 70% of pharmacists had positive views about smoking cessation and more than 50% agreed that pharmacists play an important role in motivating patients to quit [10]. Canadian pharmacists felt most strongly about their role in advising patients on the use of NRT products with more than 80% in agreement. On the other hand, the study revealed that less than 50% of those pharmacists conducted smoking cessation interventions with their patients.
A 2009 study confirmed many of the results found in the Canadian study. The smoking cessation practices of pharmacists in East Texas was assessed and findings revealed that even those individuals with knowledge of the Clinical Practice Guidelines were unlikely to use the 5 A’s (ask, advise, assess, assist, and arrange). Only 8.9% of pharmacists usually or always asked their patients about smoking cigarettes, cigars, or pipes and only 6.3% usually or always asked about smokeless tobacco products. More pharmacists (27.8%) were usually or always likely to advise patients to quit, and 62.8% were usually or always willing to assist in quitting by suggesting NRT or Zyban (bupropion). Results were similar when examining pharmacists who have received training on the 5 A’s with only 7.7% trained usually or always asking their patients about their smoking habits and 4.2% asking about smokeless tobacco use. Interestingly, when compared to pharmacists who received no training or had no knowledge of the Clinical Practice Guidelines, those trained and knowledgeable were twice as likely to usually or always practice the 5 A’s with their patients [11].
With these studies under consideration, an unanswered question is why don’t community pharmacists put forth a greater effort in counseling patients on smoking cessation? It has been suggested that pharmacist lack of emphasis of the importance of smoking cessation training in regard to pharmacologic interventions and methods of counseling may play a role [12].
Pharmacologic interventions
Studies show that the combination of counseling and medication therapy increases smoking abstinence rates [4]. There are several pharmacologic therapies available to assist patients in quitting smoking. First line medication therapies include bupropion sustained release (SR), varenicline, and nicotine gum, inhaler, lozenge, nasal spray, and patch [12]. Studies reveal that use of over the counter nicotine based medications reduces the amount of cravings that smokers experience [13,14]. Furthermore, reducing nicotine intake gradually will result in fewer withdrawal symptoms as steady doses of nicotine are received. A slow reduction in dose of nicotine over time may be achieved through patient use of nicotine replacement products. The typical usage time for these over the counter products is 12 weeks.
Patients must be counseled to understand that they cannot smoke when using these products and they must disclose any medications or allergies to avoid contraindications. Patients should not use these products if pregnant or breastfeeding. Furthermore, the following medical conditions should be disclosed by the patient to the pharmacist: asthma or breathing problems, heart or blood vessel disease, high blood pressure, stomach ulcer, diabetes mellitus, kidney disease, liver disease, overactive thyroid, or pheochromocytoma (PCC) [12,15,16].
When using the nicotine patch it should be applied directly to the skin as the nicotine passes through the skin into the bloodstream. In using the patch patients have the option of reducing the dose over time by applying different strengths. Tips on using the patch that may be provided during pharmacist counseling include: the best areas on the body to apply the patch are the upper arm or torso and the patch should not be applied to the same area within the same week, patients should ensure the area in which they apply the patch is clean and free of cuts, scars, or slippery moisturizing agents such as lotion, patients should place the pouch containing the patch aside for use in disposal of the patch, patients should never cut the patch to modify the dosage and remember the patch can work during swimming or bathing, but if it falls off, the patch should be replaced with a new patch. When using the patch common side effects include increased appetite, irritation at the application site and headache. Additionally, patients should be warned that rigorous exercise may increase the flow of nicotine from the patch into the bloodstream. Finally, the patch should be removed at night if sleep disturbances occur with use [12,15,16].
Similar to using the patch, utilization of nicotine gum allows nicotine to pass into the bloodstream, but via the lining in the mouth. Pharmacists should remind patients that they should chew only one piece of gum at a time 15 minutes apart from intake of food or drink. Gum should be chewed slowly to release the nicotine over time and gum use should be restricted only to times when the patient feels the urge to smoke. Side effects experienced with nicotine gum use include: increased appetite, nausea, jaw pain, sore throat and gas/heartburn [12,15,16].
Lastly, patients may opt to utilize an over the counter nicotine lozenge. This product is widely used by patients who enjoy hard candy. Like nicotine gum the lozenge allows nicotine to pass into the bloodstream through the lining in the mouth. Suggestions for patients include reminders that the lozenge should not be chewed and one lozenge should be taken at a time lasting for about 30 minutes. Furthermore, no more than 5 lozenges should be taken during a 6 hour timeframe and no more than 20 during 24 hours. Similar to the nicotine gum lozenges should be taken 15 minutes apart from intake of food or drink [12,15,16].
While over the counter products for smoking cessation have been shown to be effective, prescription products have been shown to be equally effective [14]. Nicotine nasal spray is a prescribed nicotine based product that is used for about 12 weeks. Pharmacists should remind patients to: reduce the dose over time by skipping doses, remember to blow the nose prior to use and note the time of day the spray is taken to reduce doses consistently over time. Side effects experienced with nicotine nasal spray include: nausea, headache, sore throat, cough, runny nose, sneezing, constipation and back pain. The spray is not suggested for people with asthma or chronic nasal disorders [12,15,16].The other prescription nicotine based product is the nicotine inhaler. While this product can be used for as long as 6 months the initial treatment period is 12 weeks and then the dose is reduced. Use of this product allows nicotine to pass from the limning of the mouth and throat to the bloodstream. Pharmacists should remind patients that the normal initial dose is about 6 to 16 cartridges per day and the inhaler should be stored in a dry area at room temperature. Furthermore, the time of day the spray is taken should be noted to reduce doses consistently over time. Common side effects include: sore throat, cough, runny nose, and indigestion [12,15,16].
Other prescription smoking cessation products include bupropion and varenicline. Bupropion is an antidepressant that might also be used to treat major depressive disorders. Pharmacists should remind patients that it takes about 2 weeks to see the effects of bupropion and therefore the smoking cessation plan should include modified smoking quit dates as appropriate. When patients take bupropion it should not be swallowed whole, crushed, or divided. Contraindications include: history of seizure disorder, bulimia, or anorexia nervosa and common side effects are dizziness, dry mouth, decreased appetite, anxiety, irritability, headache, rash and insomnia [17,18].
On the other hand, varenicline has only three common side effects including headache, nausea and insomnia. Varenicline does not contain nicotine, but works by reducing withdrawal symptoms during smoking cessation. It takes about 1 week to see the effects of varenicline. Unlike previously described products, varenicline should be taken with a glass of water and food. Several drug interactions may occur with use of other drugs including: insulin, blood thinners, and anti-asthma agents. Some studies have also revealed drug interactions with varenicline and herbal supplements [17,18].
In summary, pharmacists should inform patients to use an adequate amount of nicotine replacement therapy to assist in the process of quitting. Patients who smoke greater than ten cigarettes per day should begin with the highest dose of the nicotine patch. It is very important that patients have some form of social support when they decide to quit. Ideally, support can come from their community pharmacist. Once the appropriate smoking cessation intervention is identified an effective method for counseling must be selected.
Methods for pharmacist led smoking cessation counseling
There are two main types of smoking cessation counseling methods that can be conducted with patients, intensive or brief. Per the recommendations of the 2008 updated Clinical Practice Guidelines: Treating Tobacco Use and Dependence, intensive interventions should be used whenever possible. The guidelines state that there is a strong dose-response relationship between the session length and successful treatment outcomes. Additionally, person-to-person intensive interventions are more effective than less intensive interventions. The overall recommendation is to deliver four person-to-person treatment sessions, preferably more than four, of at least ten minutes in time length [4].
Intensive interventions have several components to increase smoking cessation rates. First, the HCP needs to assess whether a tobacco user is willing to make a quit attempt. If willing, multiple HCP types should be used. The guidelines recommend that the medical/health care clinicians deliver a strong message to quit, inform the patient about the health risks and benefits, and then recommend and/or prescribe medications for smoking cessation. Then non-medical clinicians (i.e. pharmacists) should deliver additional counseling interventions. Again, these interventions should be more than 10 minutes in length and occur at least 4 times. The follow-up interventions should then be scheduled. Individual or group counseling sessions are an option, as is telephone counseling (available at 1-800-QUIT-NOW). Self-help materials and websites are also an option. Lastly, counseling and behavioral therapies should be reinforced with medication, except when contraindicated.
Counseling should begin with the 5 A’s- ask, advise, assess, assist, and arrange follow-up. Pharmacists should begin by asking the patient if they currently use tobacco products. Most HCPs might think to ask only about use of cigarettes, but there are many tobacco products available, all of which affect the health of the patient. If the patient answers yes, they should be advised to quit, then their willingness to quit should be assessed. If they are willing, pharmacists should assist them by providing suggestions for medication and subsequent counseling. If they are unwilling, pharmacists can assist by increasing the patient’s motivation to quit using the 5 R’s- relevance (of benefits), risks (of smoking), rewards (healthier bodies, additional years of life), roadblocks (withdrawal symptoms, weight gain, fear of failure), and repetition.
Patients should also be provided with introductory information about smoking cessation and how to successfully quit. Patients should be informed that a single puff will increase the likelihood of a full relapse. Additionally, it should be mentioned that withdrawal symptoms will likely peak within one to two weeks after quitting and unfortunately can persist for months. These symptoms include, but are not limited to: negative mood, urges to smoke, and problems concentrating.
However, pharmacists should encourage patients in their quit attempts by emphasizing that one-half of all people who have ever smoked have successfully stopped. Counseling should include a discussion on the quitting process and a wrap up discussion that addresses any concerns or questions. It should also be noted that discussion of the patient’s fears, concerns, difficulties, and successes is important.
A study published in 2002 examined the effectiveness of a pharmacist based intensive counseling program on the quality of life of 31 patients who participated in the study. The intensive interventions were one-hour group meetings weekly for 12 weeks and then an additional 12 weeks for relapse prevention. Ninety-five percent of the sessions were facilitated by the same two pharmacists. During each session patients were encouraged to discuss their attempts at cessation during the previous week and were then presented a video on what to expect during the coming week. The video included techniques for behavioral modification to aid in cessation. Participants in the study used NRT, either gum or patch, for relief and prevention of withdrawal symptoms. Bupropion use was not included in this study. As such, the first session included extensive education on the NRT products including proper use and possible adverse effects. Participants chose their form of NRT based on this information and then set a quit date for the upcoming week. Within three to five days all participants were contacted by phone for additional support. Three educational courses were offered during the study with the first two being free. The third course cost patients $35 and patients were also required to pay for their NRT products. However, a discount was offered for these products if they were purchased at the outpatient pharmacy.
Results revealed, on average, 21 subjects attended each weekly session and 16 reported abstinence. Chemically verified abstinence rates were 42% at three months and 26% at six months. Vitality, mental health, self-control and quality of life were also measured at two weeks and three months. All domains showed significant improvements. In contrast to the 2008 Clinical Practice Guidelines for Treating Tobacco Use and Dependence, which recommend the use of intensive therapy, physicians achieved a six-month abstinence rate of 19.9%, while pharmacists in this study achieved a rate of 26%. While this is the result of only one study and it has not been replicated, the study provides support for the idea of pharmacist effectiveness in the provision of intensive smoking cessation counseling.
Unfortunately, other studies show that pharmacists are not partaking in intensive counseling in their community settings. One study found that only 49 of the 757 or 6.5% of patients examined were asked about their smoking habits by a pharmacist. Fewer patients were advised, assessed, assisted and received followed up. Findings revealed that physicians, however, were 5 times more likely to ask their patients about their smoking habits, 6.5 times to advice patients to quit, almost 10 times more likely to asses readiness to quit, and more than 9 times more likely to arrange a follow-up. Authors concluded that while intensive interventions were appropriate and feasible for physicians, the same finding could not be found for pharmacists.
On the other hand, a 2006 study provided contrary results. A perception and opinion study on pharmacists and tobacco cessation counseling found that 90% of 1200 pharmacist participants expressed interest in specialized training for smoking cessation and 70% believed such training would increase the number of patients they would counsel. These findings suggest that it is not a lack of interest or belief in intensive smoking cessation counseling rather a series of challenges that prevent pharmacists from being able to use the intensive method recommended by the Clinical Practice Guidelines. The challenges include little recognition and reimbursement from health care systems, lack of availability of medical records, lack of time, or unavailability of appropriate counseling areas.
In regard to brief interventions, several studies with pharmacists have been conducted to determine different modes of counseling that are best suited in a community setting. Bock and colleagues 2010, conducted a study involving a computer program, Exper_Quit (EQ). Authors divided patients into three groups, EQ, EQ plus 8 weeks of nicotine transdermal patch (EQ+), and observational. The patients in the observational group were provided a single three-hour training session with a clinical pharmacist who assessed and assisted patients with smoking cessation.
Those in the EQ and EQ+ group were asked to complete a computer provided assessment. The software provided a four-page feedback report for the patient and was designed to identify potential barriers to quitting with reinforcement of strengths. It also addressed motivation, decision making (pros and cons of quitting), triggers and cues, and the negative effects and depressive symptoms associated with cessation. A one-page report was also printed for the pharmacist, which was used to deliver brief counseling for each patient. If patients were willing to set a quit date within the following two weeks, a follow-up telephone call was scheduled for the quit date. Those in the EQ+ group were screened for appropriateness of nicotine patches and were given patches if they set a quit date. A follow up call was also scheduled at four weeks and at six months.
Results revealed that none of the participants in the observational group spoke with their pharmacist about smoking cessation. At 2 months, 27% of patients in the EQ group and 39% in the EQ+ group were abstinent, while only 9% of those in the observational group were abstinent. At 6 months, 42% of observational patients reported a quit attempt, while 76% and 65% reported an attempt in the EQ and EQ+ groups, respectively. Authors concluded that by allowing pharmacists to initiate a brief intervention, the EQ computer program produced increased quit rates and attempts for all patients involved.
Discussion
Over the past decade patient perceptions on the role of the pharmacist in smoking cessation counseling have evolved from a lack of confidence in the ability or desire of the pharmacist to provide smoking cessation counseling to an expectation of smoking cessation counseling to be provided in the community pharmacy setting. Recent discussions by pharmacist oriented organizations support a more engaging role for the pharmacist with regard to patient interaction and counseling. There is a general consensus that pharmacists of the future will need to increase patient interaction and smoking cessation counseling. The community pharmacy setting provides an ideal environment where this goal can be achieved.Currently, pharmacist knowledge on smoking cessation therapies and methods needs improvement. This study provides a summary of those therapies and methods and points toward the effective use of various methods. Several studies support the use of pharmacotherapy and behavioral therapy to assist patients in quitting smoking. Furthermore, studies show the community pharmacy setting as an ideal environment to provide such assistance. Despite evidence that supports the effectiveness of pharmacist provided smoking cessation counseling, lack of reimbursement for counseling remains a limitation. Pharmacists have not secured viable methods to ensure documentation and reimbursement for these much needed services. Although there have been advances in pharmacist reimbursement by third party payers for services provided through medication therapy management, smoking cessation related services seem to be overlooked. Perhaps pharmacists should collectively direct efforts towards highlighting the cost savings and improved patient outcomes that may be a result of pharmacist provided smoking cessation counseling. Shining a light on these value added services that pharmacists can provide may lead to greater opportunities for reimbursement.
Conclusions
Pharmacists have a unique opportunity to aid and assist patients with smoking cessation. Unlike many other HCPs, community pharmacists see patients at least once a month and are knowledgeable about over the counter and prescription smoking cessation therapies currently available. While several studies concluded that both patients and pharmacists have positive views in regard to pharmacist led smoking cessation counseling, other studies concluded that less than 10% of pharmacists ask patients about tobacco product use. This finding is in contrast to pharmacist use of the 5 A’s method for counseling which begins with ‘ask’. In the future community pharmacists will need to initiate this first step of asking patients about their tobacco use. Community pharmacists must take a different approach to counseling their patients.This includes implementing brief rather than intensive counseling sessions for all patients by assessing their willingness to quit and then motivating, educating, and referring them to an available resource. Preferably, the brief sessions should be completed in person and performed at each visit. To increase the likelihood of patient counseling, pharmacists should keep their NRT products as close to the pharmacy as possible.
Findings of this study may offer community pharmacists the necessary information to initiate smoking cessation counseling and policies for their specific setting. The role of the community pharmacist is changing with a greater focus on improving patient outcomes as opposed to increasing the number of prescriptions filled. Future research studies should focus on multidisciplinary approaches to smoking cessation and reimbursement for smoking cessation counseling. Studies on multidisciplinary approaches to smoking cessation are lacking. This is an interesting finding considering the 2008 Clinical Guidelines which stress the importance of utilization of multiple health care providers to increase quit rates. In regard to reimbursement, smoking cessation counseling has been cited as the single most cost-effective health insurance benefit for adults that can be provided to employees [19-21]. Pharmacologic interventions can double a person’s chances of quitting smoking [9]. By linking pharmacologic interventions and counseling to specific patient outcomes community pharmacists can take advantage of opportunities to help smokers achieve their goal of smoking cessation.
References
- (2012) Health Effects of Cigarette Smoking. Smoking and Tobacco Use.
- (2004) Highlights: Four Major Conclusions of the 2004 Report. Smoking and Tobacco Use.
- (1999) Achievements in Public Health, 1900-1999: Tobacco Use -- United States, 1900-1999.
- Fiore MC (2008) Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guidelines.
- (2000)Treating Tobacco Use and Dependence—A Systems Approach. A Guide for Health Care Administrators, Insurers, Managed Care Organizations, and Purchasers, U.S. Public Health Service.
- (2012) Tobacco Use. HealthyPeople.gov.
- Couchenour RL, Carson DS, Segal AR (2002) Patients’ Views of Pharmacists as Providers of Smoking Cessation Services. J Am Pharm Assoc 42: 510-512.
- Hudmon KS, Hemberger KK, Corelli RL, Kroon LA, Prokhorov AV (2003) The Pharmacist’s Role in Smoking Cessation Counseling: Perceptions of Users of Nonprescription Nicotine Replacement Therapy. J Am Pharm Assoc 43: 573-582.
- Patwardhan PD, Chewning BA (2010) Tobacco Users’ Perceptions of a Brief Tobacco Cessation intervention in community pharmacies. J Am Pharm Assoc 50: 568-574.
- Ashley MJ, Victor JC, Brewster J (2007) Pharmacists’ Attitudes, Role Perceptions and Interventions Regarding Smoking Cessation: Findings from Four Canadian Provinces. Chronic Dis Can 28: 20-28.
- Mashack A, Moultry AM, Hu S, McAlister AL (2009) Smoking Cessation Counseling Practices of Texas Pharmacists. J Community Health 35: 231-238.
- Leonard M (2006) Medications Used for Smoking Cessation. Pharmacotherapy Update from the Cleveland Clinic Department of Pharmacy Newsletter Vol. 9.
- Crain D and Bhat A (2010) Current treatment options in smoking cessation. Hosp Pract 38: 53-61.
- Corelli RL and Hudmon KS (2006) Pharmacologic interventions for smoking cessation. Crit Care Nurs Clin North Am 18: 39-51.
- Nides M (2008) Update on Pharmacologic Options for Smoking Cessation Treatment. Am J Med 121: S20-S31.
- Tom WC (2011) Smoking Cessation Drug Therapy: An Update. Pharmacist’s Letter/Prescriber’s Letter Vol. 27.
- Frishman WH (2009) Smoking cessation pharmacotherapy. Ther Adv Cardiovasc Dis 3: 287-308.
- Frishman WH (2007) Smoking cessation pharmacotherapy-nicotine and non-nicotine preparations. Prev Cardiol 10: 10-22.
- Warner KE (1997) Cost effectiveness of smoking-cessation therapies. Interpretation of the evidence and implications for coverage. Pharmacoeconomics 11: 538-549.
- Cummings SR, Rubin SM, Oster G (1989) The cost-effectiveness of counseling smokers to quit. JAMA 261: 75-79.
- Coffield AB, Maciosek MV, McGinnis JM, Harris JR, Caldwell MB, et al. (2001) Priorities among recommended clinical preventive services. Am J Prev Med 21: 1-9.