International Journal of Otorhinolaryngology
Download PDF
Case Report
*Address for Correspondence: Charles A Elmaraghy, MD, Department of Pediatric Otolaryngology, Nationwide Children’s Hospital, 700 Children’s Drive, Columbus, OH, USA, Tel: 614-722-6804; Fax: 614-722-6609; E-mail: charles.elmaraghy@nationwidechildrens.org
Citation: Fabian D, Mahida JB, Pluto CP, Thompson BP, Minneci PC, et al. Pediatric Tonsillar Malignancies: Misleading Presentations. Inter J Otorhinolaryngology. 2015;2(1): 4.
Copyright © 2015 Elmaraghy et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
International Journal of Otorhinolaryngology | ISSN: 2380-0569 | Volume: 2, Issue: 1
Submission: 07 March 2015 | Accepted: 05 May 2015 | Published: 09 May 2015
Conclusion: Appropriate imaging and careful evaluation aided in differentiating malignancy from an infections process and facilitated rapid diagnosis and institution of treatment. High index of suspicion for tonsillar malignancy is necessary for pediatric patients presenting with unilateral tonsil hypertrophy without cardinal symptoms of infection.
Case B
Pediatric Tonsillar Malignancies: Misleading Presentations
Denise Fabian1, Justin B Mahida2, Charles P Pluto3, Benjamin P Thompson3, Peter C Minneci2, Katherine J Deans2 and Charles A Elmaraghy4*
- 1The Ohio State University College of Medicine, Columbus, OH, USA
- 2Center for Surgical Outcomes Research, Nationwide Children’s Hospital, Columbus, OH, USA
- 3Division of Radiology, Nationwide Children’s Hospital, Columbus, OH, USA
- 4Department of Pediatric Otolaryngology, Nationwide Children’s Hospital, Columbus, OH, USA
*Address for Correspondence: Charles A Elmaraghy, MD, Department of Pediatric Otolaryngology, Nationwide Children’s Hospital, 700 Children’s Drive, Columbus, OH, USA, Tel: 614-722-6804; Fax: 614-722-6609; E-mail: charles.elmaraghy@nationwidechildrens.org
Citation: Fabian D, Mahida JB, Pluto CP, Thompson BP, Minneci PC, et al. Pediatric Tonsillar Malignancies: Misleading Presentations. Inter J Otorhinolaryngology. 2015;2(1): 4.
Copyright © 2015 Elmaraghy et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
International Journal of Otorhinolaryngology | ISSN: 2380-0569 | Volume: 2, Issue: 1
Submission: 07 March 2015 | Accepted: 05 May 2015 | Published: 09 May 2015
Abstract
Objective: To review a case series of pediatric patients with tonsillar malignancy presenting with symptoms similar to peritonsillar infection.Methods: We performed a chart review of patients presenting to the emergency department in 2008 with CT imaging who were diagnosed with tonsillar malignancy by otolaryngology after initial diagnosis of peritonsillar cellulitis or abscess by the emergency department. CT and MRI imaging were independently reviewed by two pediatric radiology fellows. Charts were reviewed for five years following initial diagnosis to identify evidence of recurrence.
Results: Three patients, who presented with unilateral tonsillar enlargement without fevers, dysphagia, or trismus, were initially diagnosed with peritonsillar cellulitis. Imaging studies were inconsistent with an infectious process, leading to further investigation and a final diagnosis of tonsillar malignancy. Urgent treatment precipitated recurrence-free survival in all 3 patients.
Conclusion: Appropriate imaging and careful evaluation aided in differentiating malignancy from an infections process and facilitated rapid diagnosis and institution of treatment. High index of suspicion for tonsillar malignancy is necessary for pediatric patients presenting with unilateral tonsil hypertrophy without cardinal symptoms of infection.
Keywords
Tonsillar cancer; Peritonsillar infection; Computed tomography; Magnetic resonance imagingIntroduction
Peritonsillar infections (PTA and peritonsillar cellulitis) are common neck infections in children with an incidence of 13,500 cases per year in the United States [1]. Patients with peritonsillar infections classically present with sore throat, neck pain, odynophagia, dysphagia, fever greater than 38 °C, and absent or decreased oral intake or dehydration. Physical exam findings may include neck adenopathy, uvular deviation, muffled voice, and trismus, and workup reveals leukocytosis with a left shift [2]. Due to the risk of possible infectious spread into the parapharyngeal space or deep neck spaces, airway compromise from acute enlargement, and bronchopneumonia from rupture and aspiration, urgent medical evaluation and treatment of peritonsillar infections is advised.While infectious processes of oropharyngeal and parapharyngeal tissues in the pediatric population are common, malignancies of these areas are rare. Given the greater incidence of peritonsillar infections and possible adverse sequelae, it is important to promptly recognize patients who may not present with classic clinical findings. Understandably, when the rare diagnosis of malignancy does present, it can be confused for a more common diagnosis even when a more rigorous workup with imaging is pursued.
The following is a case series of patients presenting with unilateral tonsillar enlargement in absence of fevers, dysphagia, or trismus initially diagnosed with peritonsillar cellulitis. Imaging was not consistent with an infectious process and the three patients were diagnosed with tonsillar malignancies.
Case Reports
Case AA four year old male with no significant past medical history presented with 3 weeks of sinus and nasal congestion. The patient had been referred to the otolaryngology service by his primary care physician (PCP) after noting enlarged right asymmetric posterior swelling of his posterior pharynx, which raised concerns of a peritonsillar abscess. The patient had no breathing problems, stridor, or drooling. He did not have a fever, trismus, or significantly decreased oral intake. His vital signs and leukocyte counts were within normal limits. On examination, his right tonsil was enlarged, tender, erythematous, and without exudate. He also had right anterior cervical lymphadenopathy. CT of the neck demonstrated soft tissue fullness in the posterior pharynx and right peritonsillar area without an enhancing fluid collection (Figure 1). He was diagnosed with peritonsillar cellulitis and discharged on oral clindamycin with otolaryngology follow-up a week later. After 1 week of antibiotic treatment, the patient continued to demonstrate asymmetry and the decision was made to obtain tissue for diagnosis. His pathology results indicated alveolar rhabdomyosarcoma. MRI at that time showed the lesion extending from the skull base to the pterygoids and down to the epiglottis (Figure 2). He was treated with chemotherapy with courses of vincristine, actinomycin, and cyclophosphamide and vincristine and irinotecan for 40 weeks as part of a randomized controlled clinical trial and radiation therapy. After 5 years, he is doing well with no evidence of recurrence.In addition he had right submandibular lymphadenopathy. CT of the neck showed a 2x2 cm right parapharyngeal soft tissue swelling, thought to be consistent with a possible peritonsillar phlegmon (Figure 1). His vital signs and leukocyte counts were within normal limits. He was admitted to the infectious disease service and started on intravenous clindamycin. No improvement was noted withantibiotic treatment after 2 days, and the decision was made to proceed with operative intervention Consent was obtained and the patient underwent a tonsillectomy and excisional biopsy of a firm tonsillar mass that extended into the parapharyngeal space. He was diagnosed with stage III Burkitt’s lymphoma. He underwent systemic chemotherapy with vincristine, dactomycin, methotrexate, and Cytoxan and has no evidence of recurrence five years after treatment.
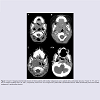
Figure 1: Axial CT imaging of peritonsillar lesions for three patients with tonsillar malignancies and a patient with a peritonsillar abscess. Panels “A”, “B”, and “C” are CT images of patient case A, B, and C, respectively. Panel “PTA” is an image from a patient with a peritonsillar abscess. White arrowheads point to the tonsillar malignancy or peritonsillar abscess.
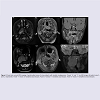
Figure 2: Axial and coronal MRI imaging of peritonsillar lesions for two patients with tonsillar malignancies. Panels “A” and “C” are MRI images of patient case A and C, respectively. Panel “1” shows T2-weighted axial images. Panel “2” shows T1-weighted axial images. Panel “3” shows T1-weighted coronal images.
A three year old male with a 2 week history of decreased oral intake and malaise presented to his PCP with a sore throat. He had not been behaving normally and was complaining of ear pain and a muffled voice. His parents denied evidence of fever, trismus, or headaches associated with his symptoms. His primary care physician referred him for a possible peritonsillar abscess. Examination revealed enlargement of his right tonsil and surrounding soft palate.
Case C
An eight year old male presented with a 1 week history of sore throat and increasingly muffled voice. He had no history of fevers or decreased oral intake. However, he did have new onset snoring. He presented to an outside hospital where he was presumed to have a right peritonsillar abscess. He received oral clindamycin and was transferred to our institution. Examination revealed bilateral tonsillar erythema with exudates, right soft palatal swelling with uvular deviation, and right superior cervical tender lymphadenopathy to level II. Further examination later appreciated tongue deviation to the right and mild right eye ptosis, suggesting Horner’s syndrome and a hypoglossal defect. CT of the neck showed a low density area in the right palatine tonsil with extensive right parapharyngeal soft tissue swelling exerting a mass effect on the airway (Figure 1). MRI confirmed a large mass in the right parapharyngeal region (Figure 2). Excisional biopsy of the mass was consistent with Burkitt’s lymphoma. He received a tonsillectomy and adenoidectomy along with chemotherapy treatment involving systemic vincristine, methotrexate, doxorubicin, and Cytoxan in addition to intrathecal methotrexate. He has no evidence of disease recurrence after 5 years.
Discussion
The differential diagnosis for patients with a suspected peritonsillar infection includes epiglottitis, supraglottitis, jugular venous thrombosis, peritonsillar cellulitis, retropharyngeal abscess, parapharyngeal abscess, supraglottitis, and malignancy including cancer of the palatine tonsil. Compared to oropharyngeal infections, cancer of the palatine tonsil is rare. Discovery of clinically relevant disease in routine tonsillectomy specimens is very rare: in one study, the reported incidences of unexpected clinically relevant diagnoses varied between 0.0% and 0.05% [3].A patient with a tonsillar malignancy can present with a neck mass, weight loss, systemic symptoms of night sweats, and lethargy, prior history of cancer, presence of a firm tonsillar lesion, and asymmetry of the palatine tonsils. As with our three cases, patients do not present with infectious signs or symptoms such as fever. Of note, tonsillar asymmetry without classic symptoms such as progressive enlargement of the tonsil, significant systemic signs, or history of malignancy is associated with but not pathognomonic for tonsillar cancer [4]. A recent review of the literature by Guimarães in 2015 corroborated this finding the most common clinical presentations for tonsillar malignancy were unilateral tonsillar enlargement (72.7%), alterated appearance of the tonsil (45.4%) and cervical lymphadenopathy (30.3%). Presence of B symptoms was rare and occurred in only 16% of the patients. Burkitt was the most common type of lymphoma found [5]. The majority of pediatric patients with unilateral tonsillar enlargement will not have a malignancy; however, patients with a malignancy will most likely have unilateral tonsillar enlargement as a presenting symptom. Therefore, close follow-up of these patients is essential to avoid disastrous sequelae of missing or prolonging diagnosis [4]. Patients with atypical symptoms that do not respond rapidly to antibiotics should undergo imaging; if imaging does not suggest abscess or cellulitis, then additional evaluation including either an MRI and or biopsy is warranted. Workup is based on clinical exam findings, and controversy exists with regards to use of imaging, but one purpose of imaging is to differentiate infection from tonsillar malignancy in patients with atypical presentations. Recent studies have cautioned clinicians using CT imaging in children due to potential risk of radiation induced malignancy [6]. Alternatively, CT imaging enhances diagnostic accuracy in distinguishing abscesses from cellulitis [7] and reduces morbidity by eliminating unnecessary drainage of peritonsillar cellulitis [8]. In all three cases, subtle findings on CT imaging with contrast were inconsistent with a diagnosis of infection and prompted further evaluation for tonsillar malignancy. Abscess typically appears on CT imaging as a hypodense mass with ring enhancement (Figure 1). Findings consistent with peritonsillar cellulitis include soft tissue swelling, loss of surrounding fat planes, and lack of ring enhancement. In our case series, all three lesions resembled phlegmons or cellulitis on CT imaging, but were surprisingly large and with mass effect or ring enhancement. Additionally, no inflammatory fat stranding surrounding the lesions was noted.
Although most cases of peritonsillar infection are relatively straightforward on CT, the superior contrast resolution of MRI provides better delineation of tissue planes, allowing better determination of exact anatomical location and extension (Figure 2). In patients with malignancy, the extent of involvement needs to be determined for staging or pre-surgical planning. For these reasons, two of the three patients underwent further imaging with MRI. Two important features that cannot be adequately assessed with CT imaging alone are extension into the neural foramina and spinal canal and perineural spread of tumor along cranial nerves. Although CT has the advantage of being relatively fast (in cases of possible airway compromise) and is usually adequate in characterizing PTA, MRI has the advantage of increased soft tissue contrast resolution as well as no ionizing radiation. Choice of imaging modality should take into consideration the need for rapid diagnosis, the potential need for sedation in pediatric patients for MRI, and airway concerns.
In our case series, two patients presented with Burkitt’s lymphoma and one presented with rhabdomyosarcoma. Lymphoma (59%) and rhabdomyosarcoma (13%) are the most frequent head and neck cancers in children. Other pediatric cancers found in this region include thyroid carcinoma, nasopharyngeal carcinoma, neuroblastoma, nonrhabdomyosarcoma, and salivary gland malignancies [9]. Most adult oropharyngeal cancers, in contrast, are squamous cell carcinomas (SCC) [10]. Rhabdomyosarcoma (RMS) is the most common soft tissue sarcoma and accounts for 7% of all pediatric malignancies [11]. Evaluation involves staging studies that include CT or MRI of the primary site, bone scan, chest CT, and bilateral bone marrow aspirate and biopsy. The success of MRI determining soft tissue mass as benign or malignant is between 30-90% depending on study population. MRI is also essential for determining the resectability of lesions. Lymphoma represents 11.5% of all pediatric cancer. Non-Hodgkin’s lymphoma (NHL) account for roughly 7% of all pediatric cancer [12]. NHL is classified into three subgroups: mature B-cell lymphoma, which includes Burkitt’s lymphoma, diffuse large B cell, and mediastinal large B cell lymphomas; lymphoblastic lymphoma; and anaplastic large cell lymphoma [13]. Extra nodal localizations of NHL include initial presentations in the parapharyngeal lymphoid ring Waldeyer’s ring, with the tonsil being the most frequent site [14]. Initial workup involves hematologic studies, imaging studies, and cytological evaluation.
The survival of patients with tonsillar malignancies is dependent on early diagnosis and treatment. For RMS, overall 5-year survival for patients with local disease is 75%, whereas patients with metastatic disease have a 5-year survival rate of only 24% [15]. Metastases are present in 10-20% at the time of diagnoses, most commonly involving the lung, bone, lymph nodes, bone marrow, and liver [16]. NHL prognosis is based on the stage of the disease with survival rates between 65-85%. Clinically, the presence of lymphadenopathy for greater than 4 weeks duration, greater than 3 cm in size, and/or with supraclavicular involvement should increase suspicion for malignancy. Treatment of RMS includes a combination of surgery, radiation therapy and chemotherapy [17]. In contrast, chemotherapy is the standard treatment for NHL; radiation is not routinely used as with Hodgkin’s lymphoma. In NHL, surgical intervention is usually pursued to obtain a biopsy for diagnostic purposes [18]. In our case series, all three patients were diagnosed and treated promptly and none had disease recurrence or significant morbidity at 5 years.
Conclusion
For patients presenting with unilateral tonsillar enlargement without signs and symptoms of a peritonsillar infection, high index of suspicion should be maintained for malignancy. Prompt diagnosis involves appropriate imaging and biopsy for patients with clinical course consistent with malignancy.Acknowledgements
This work was presented at the 113th Annual Meeting of the Triological Society, Las Vegas, Nevada, USA, April 30-May 1, 2010.Funding Support: This project is supported by intramural funding from the Department of Otolaryngology and the Center for Surgical Outcomes Research at Nationwide Children’s Hospital.
References
- Jaryszak E, Choi S (2012) Deep Neck Space Infections, in Schoem SR and Darrow DH (eds): Pediatric Otolaryngology. Elk Grove Village, IL, Am Acad Pediatr, pp. 272-299.
- Nagy M, Backstrom J (1999) Comparison of the sensitivity of lateral neck radiographs and computed tomography scanning in pediatric deep‐neck infections. Laryngoscope 109: 775-779.
- Stone ME, Walner DL, Koch BL, Egelhoff JC, Myer CM (1999) Correlation between computed tomography and surgical findings in retropharyngeal inflammatory processes in children. Int J Pediatr Otorhinolaryngol 49: 121-125.
- Elden LM, Grundfast KM, Vezina G (2001) Accuracy and usefulness of radiographic assessment of cervical neck infections in children. J Otolaryngol 30: 82-89.
- Fédérici S, Silva C, Maréchal C, Laporte E, Sévely A, et al. (2009) Retro- and parapharyngeal infections: standardization of their management. Arch Pediatr 16: 1225-1232.
- Vural C, Gungor A, Comerci S (2003) Accuracy of computerized tomography in deep neck infections in the pediatric population. Am J Otolaryngol 24: 143-148.
- Nagy M, Pizzuto M, Backstrom J, Brodsky L (1997) Deep neck infections in children: a new approach to diagnosis and treatment. Laryngoscope 107: 1627-1634.
- Boucher C, Dorion D, Fisch C (1999) Retropharyngeal abscesses: a clinical and radiologic correlation. J Otolaryngol 28: 134-137.
- Daya H, Lo S, Papsin BC, Zachariasova A, Murray H, et al. (2005) Retropharyngeal and parapharyngeal infections in children: the Toronto experience. Int J Pediatr Otorhinolaryngol 69: 81-86.
- Kliegman R, Nelson WE (2011) Nelson textbook of pediatrics. Philadelphia, PA, Elsevier/Saunders.
- McClay JE, Murray AD, Booth T (2003) Intravenous antibiotic therapy for deep neck abscesses defined by computed tomography. Arch Otolaryngol Head Neck Surg 129: 1207-1212.
- Wong DK, Brown C, Mills N, Spielmann P, Neeff M (2012) To drain or not to drain - management of pediatric deep neck abscesses: a case-control study. Int J Pediatr Otorhinolaryngol 76: 1810-1813.
- Craig FW, Schunk JE (2003) Retropharyngeal abscess in children: clinical presentation, utility of imaging, and current management. Pediatrics 111: 1394-1398.
- Bolton M, Wang W, Hahn A, Ramilo O, Mejias A, et al. (2013) Predictors for successful treatment of pediatric deep neck infections using antimicrobials alone. Pediatr Infect Dis J 32: 1034-1036.
- Al-Sabah B, Bin Salleen H, Hagr A, Choi-Rosen J, Manoukian JJ, et al. (2004) Retropharyngeal abscess in children: 10-year study. J Otolaryngol 33: 352-355.
- Page C, Biet A, Zaatar R, Strunski V (2008) Parapharyngeal abscess: diagnosis and treatment. Eur Arch Otorhinolaryngol 265: 681-686.
- Maroldi R, Farina D, Ravanelli M, Lombardi D, Nicolai P (2012) Emergency imaging assessment of deep neck space infections. Semin Ultrasound CT MR 33: 432-442.
- Hoffmann C, Pierrot S, Contencin P, Morisseau-Durand MP, Manach Y, et al. (2011) Retropharyngeal infections in children. Treatment strategies and outcomes. Int J Pediatr Otorhinolaryngol 75: 1099-1103.
- Cheng J, Elden L (2013) Children with deep space neck infections: our experience with 178 children. Otolaryngol Head Neck Surg 148: 1037-1042.
- Strom DJ, Cameron JR (2002) Is it useful to assess annual effective doses that are less than 100 mSv? Radiat Prot Dosimetry 98: 239-245.
- (2007) The 2007 Recommendations of the International Commission on Radiological Protection. ICRP publication 103. Annals of the ICRP 37: 1-332.
- Stone R (2001) Living in the Shadow of Chernobyl. Science 292: 420-426.
- Huda W, Atherton JV, Ware DE, Cumming WA (1997) An approach for the estimation of effective radiation dose at CT in pediatric patients. Radiology 203: 417-422.
- Smith-Bindman R, Lipson J, Marcus R, Kim KP, Mahesh M, et al. (2009) Radiation dose associated with common computed tomography examinations and the associated lifetime attributable risk of cancer. Arch Int Med 169: 2078-2086.
- Mazonakis M, Tzedakis A, Damilakis J, Gourtsoyiannis N (2007) Thyroid dose from common head and neck CT examinations in children: is there an excess risk for thyroid cancer induction? Eur Radiol 17: 1352-1357.
- Wang B, Gao BL, Xu GP, Xiang C (2013) Images of deep neck space infection and the clinical significance. Acta Radiol 55: 945-951.