Journal of Orthopedics & Rheumatology
Total Knee Arthroplasty with a Lateral Centre of Rotation Design Retained Native Knee Joint Kinematics: A Cadaveric Study under Simulated Muscle Loads
Karsten Engel1*, Katina Mira Fischer1, Gert-PeterBrüggemann1 and Christian Liebau2
- 1Institute of Biomechanics and Orthopedics, German Sport University Cologne, Germany
- 2Asklepios Harzklinik, Germany
*Address for Correspondence: Karsten Engel, Institute of Biomechanics and Orthopedics, German Sport University of Cologne, Am Sportpark Müngersdorf 6, 50933 Cologne, Germany, Tel: +49 (0) 221 - 4982 7630/+49; Fax: +49 (0) 221 - 4971598; E-mail: k.engel@dshs-koeln.de
Citation: Engel K, Fischer KM, Brüggemann GP, Liebau C. Total Knee Arthroplasty with a Lateral Centre of Rotation Design Retained Native Knee Joint Kinematics: A Cadaveric Study under Simulated Muscle Loads. J Orthopedics Rheumatol. 2016; 3(1): 6.
Copyright © 2016 Engel K, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Orthopedics & Rheumatology | ISSN: 2334-2846 | Volume: 3, Issue: 1
Submission: 15 December 2015 | Accepted: 22 February 2016| Published: 27 February 2016
Abstract
Background: Since controversial results on the location of the centre of rotation in the native human knee joint exist, it is still unclear how the design of a total knee replacement should be in order to retain patients’ knee joint movement after Total knee Arthroplasty. Therefore, the aim of the present study was to determine individual native tibiofemoral joint kinematics as well as the centre of rotation and to investigate the influence of a total knee implant with a proposed lateral centre of rotation on the knee kinematics.Introduction
The goal of a Total Knee Arthroplasty (TKA) is to relieve pain and ideally to regain the individual tibiofemoral joint kinematics. However, patients’ satisfaction after TKA ranges between 70% and 90% [1-3], which might be associated with the different available implant designs and thus, in turn, with ongoing discussion on the kinematics of the native human tibiofemoral joint [4-6]. In addition to cruciate substituting, cruciate retaining, mobile or fixed bearing designs, differentiation with regards to the location of the pivot, or more precisely with the centre of rotation (COR) of the knee joint, has to be taken into account. Knee implants with a medial COR design as well as implants with a lateral one can be found in several studies [7-11]. The presence of the COR in the medial compartment was explained by the high congruence of the femoral epicondyle with the concave medial tibia surface and has been accepted for years [12-14], whereas more recent studies obtained controversial results. During walking and dynamic activities a COR on the lateral compartment was found [15-17], while during squats and kneeling a COR on the medial side was described [18-20]. In contrast to this activity dependent motion pattern, it was found that the COR could be medial or lateral, depending not on the activity but on the individual person [21].Materials and Methods
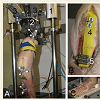
Dynamic squats driven by simulated muscle forces were carried out in a custom - made knee joint loading simulator (Figure 1A). The kinematics of the intact native tibiofemoral joint (NJ condition) as well as it’s COR were determined as a reference condition. During the experiments a Total Knee Arthroplasty using an implant with a lateral COR (TKA condition) was conducted to successively study the influences on the rotational and translational tibiofemoral joint kinematics. The Ethics Committee of the German Sport University approved the study. The specimens were provided by the Anatomical Institute I, University of Erlangen, Germany and written informed consents of the donors were given for use of this sample in medical research.The thighs were amputated 300 mm above the knee joint lines, whereas the foot and ankle complexes were kept intact to restore the native individual tibia anatomy and thus the kinematics in the closed kinematic chain. In order to simulate the entire quadriceps muscle, a 15 mm wide polyester band was used. Therefore, an incision from 50 mm above the patella to approximately 30 mm below the tibial tuberosity was done to set a casing clamp near the tibial insertion of the patella ligament as a support for the polyester band (Figure 1B). This was centrally aligned to the tibial tuberosity, centre-fixed onto the patella and passed through on top of the rectus femoris muscle to the proximal end of the thigh. The skin in front of the knee was closed using sutures. An aluminium tube was fixed to the proximal and of the femur to create a connection to the sliding bar of the knee joint loading simulator, which is described in detail in a later section.
Results
The individual rotational kinematics of all nine investigated specimens revealed a great variance with regards to the direction of rotation and in the amplitude (Figure 2). Most of the knee joints showed slight tibial rotations relative to the femurs, from 10° to 60° of flexion. Only three joints had greater internal rotations of the tibiae at 60° of flexion, with a gradual increase from the extended joint. Interestingly, the knee joints of one donor (SP3 and SP4) showed external rotations of up to -6° during the flexion cycle.In order to have a better comparison of the tibial rotation between the different experimental conditions, three cases (SP1,SP3,SP6) were chosen as representative examples of all the investigated specimens. In general, total knee replacement did not change the rotational tibiofemoral kinematic pattern in comparison to the native condition (Figure 3). The differences due to the TKA varied between the investigated specimens, although the overall trend was consistent.
Small differences were found between 10° and 30° of flexion for SP1, whereas greater changes were revealed in the range up to 60° resulting in a difference of 3°. As shown in Figure 3, the impact of the TKA was higher in the flexion range between 10° and 30° for the other two specimens. The difference became smaller with increasing flexion angle, leading to almost the same tibial rotation angle at 60° of flexion.As with the rotational kinematics, a high variance was also found for the translations (Table 1). During the extension - flexion cycles the anterior - posterior translation of the medial epicondyle was in a range between 3 mm and 9 mm in the NJ condition. The translation of the lateral epicondyle ranged from 4 mm to 20 mm in the same experimental condition.
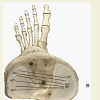
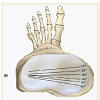
In comparison to the NJ condition, greater translations of up to 6 mm were found for the medial epicondyle in the TKA condition, except in one specimen. Four of the nine specimens revealed decreased femoral translation between 2 mm and 12 mm on the lateral side compared to the NJ condition. An increased lateral translation of between 3 mm and 8 mm was found in three knee joints, whereas two did not show any translational changes.The calculated COR was found on the medial side of the tibia plateau in eight specimens in the intact native joint condition (Table 1 and Figure 4). Just one knee joint showed a lateral COR. In seven cases the centre was outside of the tibia plateau. A lateral COR was found in five cases for the TKA condition (Table 1 and Figure 5). Interestingly, both knee joints performing an external rotation of the tibia during flexion as well as two joints with a large translation in the NJ condition remained with a medial COR.
Discussion
The chosen approach in the present study represents the first direct measurement of three dimensional tibiofemoral joint kinematics to successively investigate the effects of a TKA with a proposed lateral COR on rotational and translational knee joint kinematics as well as on the COR in comparison to the native condition. The demand for more physiological experimental conditions [22] in cadaveric studies was met by including the individual anatomy of the ankle joint in a closed kinematic chain experiment. Therefore, presentation of the individual data was chosen instead of averaged motion patterns.Acknowledgements
We thank Prof. Dr. Neuhuber and Dr. Buder from Anatomical Institute I, University of Erlangen, for their support and for providing the specimens. Our great thanks belong to Martin Küsel and Jürgen Geiermann for technical aid. Also many thanks to PD Dr. Jens Dargel from the Clinic for Orthopaedics and Trauma Surgery, University of Cologne for his comments on the manuscript.References
- Noble PC, Gordon MJ, Weiss JM, Reddix RN, Conditt MA, et al. (2005) Does total knee replacement restore normal knee function? Clin Orthop Relat Res: 157-165.
- Noble PC, Conditt MA, Cook KF, Mathis KB (2006) The john insall award: patient expectations affect satisfaction with total knee arthroplasty. Clin Orthop Relat Res 452: 35-43.
- Kessler S, Käfer W (2007) Comparative assessment of outcome in osteoarthritis of the knee: the utility of knee scores. Acta Chir Orthop Traumatol Cech 74: 332-335.<
- Tanzer M, Smith K, Burnett S (2002) Posterior-stabilized versus cruciate-retaining total knee arthroplasty: balancing the gap. J Arthroplasty 17: 813-819.
- Chalidis BE, Sachinis NP, Papadopoulos P, Petsatodis E, Christodoulou AG, et al. (2011) Long-term results of posterior-cruciate-retaining Genesis I total knee arthroplasty. J Orthop Sci 16: 726-731.
- Parsley BS, Conditt MA, Bertolusso R, Noble PC (2006) Posterior cruciate ligament substitution is not essential for excellent postoperative outcomes in total knee arthroplasty. J Arthroplasty 21 (6 Suppl 2): 127-131.
- Ishida K, Matsumoto T, Tsumura N, Chinzei N, Kitagawa A, et al. (2012) In vivo comparisons of patellofemoral kinematics before and after ADVANCE Medial-Pivot total knee arthroplasty. Int Orthop 36: 2073-2077.
- Hossain F, Patel S, Rhee SJ, Haddad FS (2011) Knee arthroplasty with a medially conforming ball-and-socket tibiofemoral articulation provides better function. Clin Orthop Relat Res 469: 55-63.
- Moonot P, Mu S, Railton GT, Field RE, Banks SA (2009) Tibiofemoral kinematic analysis of knee flexion for a medial pivot knee. Knee Surg Sports Traumatol Arthrosc 17: 927-934.
- Digennaro V, Zambianchi F, Marcovigi A, Mugnai R, Fiacchi F, et al. (2014) Design and kinematics in total knee arthroplasty. Int Orthop 38: 227-233.
- Watanabe T, Ishizuki M, Muneta T, Banks SA (2013) Knee kinematics in anterior cruciate ligament-substituting arthroplasty with or without the posterior cruciate ligament. J Arthroplasty 28: 548-552.
- Elias SG, Freeman MA, Gokcay EI (1990) A correlative study of the geometry and anatomy of the distal femur. Clin Orthop Relat Res 260: 98-103.
- Todo S, Kadoya Y, Moilanen T, Kobayashi A, Yamano Y, et al. (1999) Anteroposterior and rotational movement of femur during knee flexion. Clin Orthop Relat Res 362: 162-170.
- Iwaki H, Pinskerova V, Freeman MA (2000) Tibiofemoral movement 1: the shapes and relative movements of the femur and tibia in the unloaded cadaver knee. J Bone Joint Surg Br 82: 1189-1195.
- Koo S, Andriacchi TP (2008) The knee joint center of rotation is predominantly on the lateral side during normal walking. J Biomech 41: 1269-1273.
- Hoshino Y, Tashman S (2012) Internal tibial rotation during in vivo, dynamic activity induces greater sliding of tibio-femoral joint contact on the medial compartment. Knee Surg Sports Traumatol Arthrosc 20: 1268-1275.
- Kozanek M, Hosseini A, Liu F, Van de Velde SK, Gill TJ, et al. (2009) Tibiofemoral kinematics and condylar motion during the stance phase of gait. J Biomech 42: 1877-1884
- Asano T, Akagi M, Tanaka K, Tamura J, Nakamura T (2001) In vivo three-dimensional knee kinematics using a biplanar image-matching technique. Clin Orthop Relat Res 388: 157-166.
- Yamaguchi S, Gamada K, Sasho T, Kato H, Sonoda M, et al. (2009) In vivo kinematics of anterior cruciate ligament deficient knees during pivot and squat activities. Clin Biomech (Bristol, Avon) 24: 71-76.
- Moro-oka TA, Hamai S, Miura H, Shimoto T, Higaki H, et al. (2008) Dynamic activity dependence of in vivo normal knee kinematics. J Orthop Res 26: 428-434.
- Komistek RD, Dennis DA, Mahfouz M (2003) In vivo fluoroscopic analysis of the normal human knee. Clin Orthop Relat Res: 69-81.
- Varadarajan KM, Harry RE, Johnson T, Li G (2009) Can in vitro systems capture the characteristic differences between the flexion-extension kinematics of the healthy and TKA knee? Med Eng Phys 31: 899-906.
- Kamath AF, Israelite C, Horneff J, Lotke PA (2010) Editorial: What is varus or valgus knee alignment?: a call for a uniform radiographic classification. Clin Orthop Relat Res 468: 1702-1704.
- Banks SA, Hodge WA (2004) 2003 Hap Paul Award paper of the International Society for Technology in Arthroplasty. Design and activity dependence of kinematics in fixed and mobile-bearing knee arthroplasties. J Arthroplasty 19: 809-816.
- D'lima DD, Poole C, Chadha H, Hermida JC, Mahar A, et al. (2001) Quadriceps moment arm and quadriceps forces after total knee arthroplasty. Clin Orthop Relat Res 392: 213-220.
- Yildirim G, Walker PS, Boyer J (2009) Total knees designed for normal kinematics evaluated in an up-and-down crouching machine. J Orthop Res 27: 1022-1027.
- Churchill DL, Incavo SJ, Johnson CC, Beynnon BD (1998) The transepicondylar axis approximates the optimal flexion axis of the knee. Clin Orthop Relat Res 356: 111-118.
- More RC, Karras BT, Neiman R, Fritschy D, Woo SL, et al. (1993) Hamstrings--an anterior cruciate ligament protagonist: An in vitro study. Am J Sports Med 21: 231-237.
- D'Lima DD, Trice M, Urquhart AG, Colwell CW Jr (2000) Comparison between the kinematics of fixed and rotating bearing knee prostheses. Clin Orthop Relat Res 380: 151-157.
- Patil S, Colwell CW Jr, Ezzet KA, D'Lima DD (2005) Can normal knee kinematics be restored with unicompartmental knee replacement? J Bone Joint Surg Am 87: 332-338.
- Harman MK, Bonin SJ, Leslie CJ, Banks SA, Hodge WA (2014) Total knee arthroplasty designed to accommodate the presence or absence of the posterior cruciate ligament. Adv Orthop 2014: 178156.
- Barnes CL, Blaha JD, DeBoer D, Stemniski P, Obert R, et al. (2012) Assessment of a medial pivot total knee arthroplasty design in a cadaveric knee extension test model. J Arthroplasty 27: 1460-1468.
- Müller O, Lo J, Wünschel M, Obloh C, Wülker N (2009) Simulation of force loaded knee movement in a newly developed in vitro knee simulator. Biomed Tech (Berl) 54: 142-149.
- Escamilla RF, Fleisig GS, Zheng N, Barrentine SW, Wilk KE, et al. (1998) Biomechanics of the knee during closed kinetic chain and open kinetic chain exercises. Med Sci Sports Exerc 30: 556-569.
- Isear JA Jr, Erickson JC, Worrell TW (1997) EMG analysis of lower extremity muscle recruitment patterns during an unloaded squat. Med Sci Sports Exerc 29: 532-539.