Journal of Hematology & Thrombosis
Download PDF
Research Article
Survival of Patients with Hematologic Malignancies and Covid-19
Gilberto BL1, Yubelka BM1, Carlos MM1, Humberto CS1, Christian RP1, Francisco ZP1, Estrada Manuel DM1, Marino O1, Efreén M1, Karla R1, Adolfo M2, Irma O2 and Mónica B3
1Department of Hematology, Hospital General de México Dr.
Eduardo Liceaga
2Molecular biology laboratory, Hospital General de México Dr.
Eduardo Liceaga
3Department of Nutrition, Hospital General de México Dr. Eduardo
Liceaga
*Address for Correspondence:
Gilberto BL, Department of Hematology, Hospital General de
México Dr. Eduardo Liceaga Email: domcrupi@gmail.com
Submission: 08 May, 2022
Accepted: 08 June, 2022
Published: 10 June, 2022
Copyright: © 2022 Gilberto BL, et al. This is an open access article
distributed under the Creative Commons Attribution License, which
permits unrestricted use, distribution, and reproduction in any medium,
provided the original work is properly cited.
Abstract
Purpose: The present study aimed to describe the characteristics
of patients with hematological neoplasms and COVID19, treated in a
reference center in Mexico City, as well as their mortality and the factors
that could influence it.
Patients and methods: This retrospective study included 56 patients
with hematological neoplasms and SARS-CoV-2 infection. The impact
on overall survival (OS) of sex, age, malignancy status, diabetes mellitus,
obesity, overweight, neutrophil count, lymphocyte count, CO-RADS was
evaluated.
Results: Overall mortality was 50%. Univariate analysis identified age
>50 years, history of hypertension, diabetes, and a CO-RADS score >5 as
factors influencing the mortality of patients with hematologic malignancies
and COVID19. Multivariate analysis only identified CO-RADS score > 5.
Conclusion: The mortality of patients with hematological neoplasms
and COVID19 was high in our setting. Frequent co morbidities in our
population can influence mortality.
Keywords
SARS-CoV-2; Hematology; COVID-19; Hematological
diseases
Introduction
COVID19, caused by the SARS-CoV-2 virus, was declared
a pandemic by the WHO in March 2020. Since then, multiple
questions have arisen related to the prognosis and care of cancer
patients. Initially, recommendations formulated by groups of experts
were issued in order to guide the care of patients with hematological
neoplasms and COVID19; subsequently, the experience of various
regions of the planet was published, with variable mortality rates
[1-4].
Various risk factors have been described that can influence the
mortality of patients with hematological neoplasms and COVID19,
such as age, type of neoplasm, comorbidities, certain laboratory
parameters, etc [5,6].
The objective of this work is to describe the characteristics of
patients with hematological neoplasms and COVID19, treated in a
reference center in Mexico City, as well as their mortality and the
factors that could influence it.
Methods
We include patients with hematological neoplasms and SARSCoV-
2 infection, corroborated by the polymerase chain reaction
(PCR) test, which required hospitalization at the Hospital of Mexico
Dr. Eduardo Liceaga between April 2020 and March 2021.
The primary analysis describes the demographic and clinical
characteristics of patients with COVID19 after a previous diagnosis
of hematologic malignancy. Categorical variables are presented with
frequencies and percentages, and continuous variables with median and range. The secondary analysis studied the independent predictors
of overall mortality in hematological patients with COVID-19, using
a Cox proportional hazard model. A univariate Cox regression model
was performed with variables suspected of playing a role in the mortality
of patients with hematologic malignancies with COVID-19 (i.e., sex
[reference woman], age [<50 years of reference], malignancy status
[reference controlled disease], diabetes mellitus, obesity, overweight,
neutrophils [reference >0.5 x 109/L], lymphocytes [reference > 0.2 x
109/L], CO-RADS [<5 reference]). Variables with a p value ≤ 0.1 were
considered for multivariate analysis. A multivariate Cox regression
model was calculated, and only those variables that were statistically
significant were shown. Mortality was analyzed using Kaplan-Meier
survival graphs. No a priori sample size calculation was performed
for this exploratory study. SPSSv25.0 (SPSS, IBM CorpChicago, IL,
United States) was used for statistical analyzes.
Results
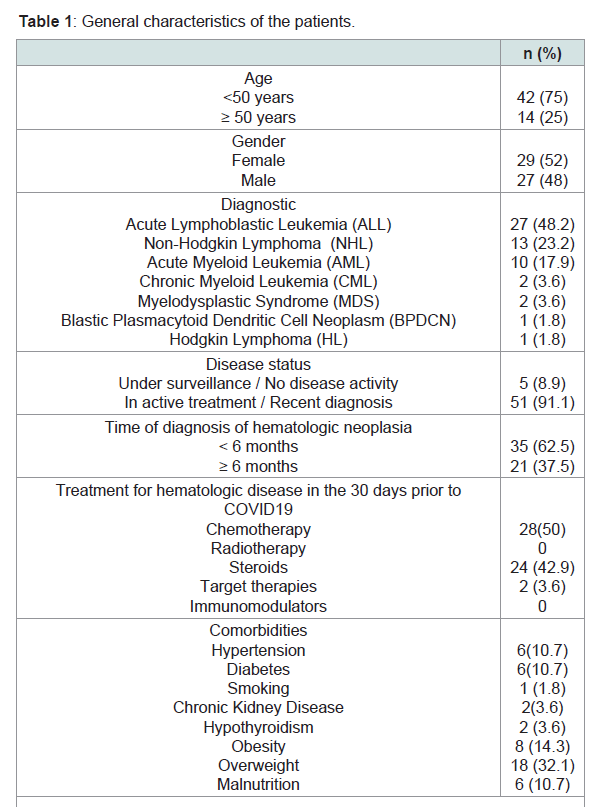
A total of 56 patients with some hematological neoplasms and
SARS-CoV-2 infection that required hospitalization were included,
with a mean age of 39 years and a predominance of males. The most
frequent diagnosis was Acute Lymphoblastic Leukemia (ALL),
followed by Non-Hodgkin’s Lymphoma (NHL) and Acute Myeloid
Leukemia (AML) (Table 1).
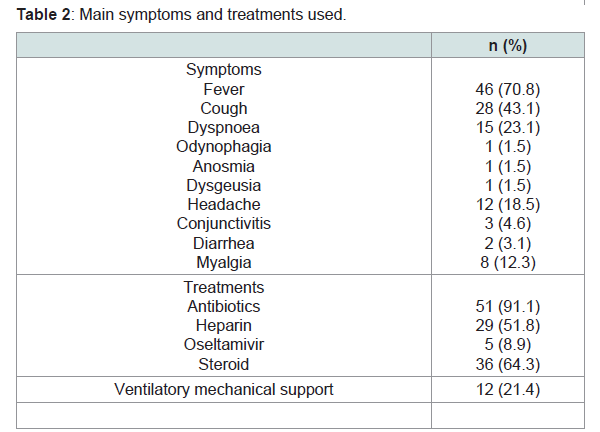
The main symptoms at diagnosis of COVID-19 were fever
(70.8%), cough (43.1%) and dyspnea (23.1%). 91% of the patients
received treatment with antibiotics and supplemental oxygen,
21% assisted mechanical ventilation, the rest of the treatments are
described in Table 2.
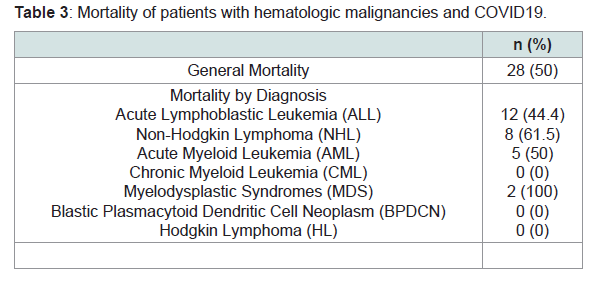
Mortality:
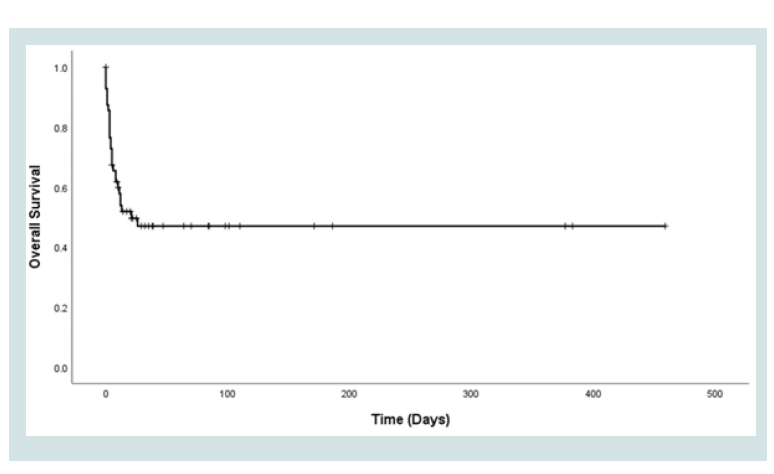
Mortality was 50% with a median survival of 21 days (Figure 1).
The highest mortality was observed in patients with non-Hodgkin’s
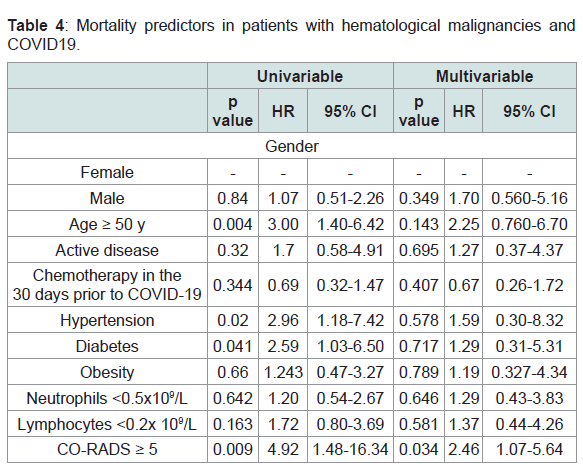
lymphoma (61.5%). Mortality by diagnosis is described in Table 3.Univariate analysis identified age ≥ 50 years (HR=3.00, CI 1.40-
6.42, p=0.004), history of hypertension (HR= 2.96, CI 1.18-7.42,
p=0.02), diabetes (HR= 2.59, CI 1.03-6.5, p= 0.02), and a CO-RADS
score ≥ 5 (4.92, CI 1.48-16.34, p=0.009) as factors associated with
mortality. In the multivariate analysis, only the CO-RADS score ≥5
(HR 2.46, CI 1.07-5.64, p=0.034) was identified (Table 4).
Discussion
Coronavirus disease 2019 (COVID-19) was declared a global
pandemic by the World Health Organization (WHO) on 11 March
2020 [7]. As the disease spread worldwide, uncertainty arose about the
treatment and prognosis of patients with hematologic malignancies.
At the beginning, only recommendations from groups of experts
were published, currently we have evidence from different parts of
the world. As of today (May 17, 2022), 522,278,953 cases of COVID
19 have been reported in the world population, with a mortality of
1.2%. In Mexico, 5,752,441 cases of COVID-19 have been reported in
the general population, with a mortality of 5.6% [8].
In the case of patients with hematological neoplasms, different
mortality ranges have been reported, for example, a multicenter
study of the Spanish transplant group and cell therapy (GETH) in
which 367 patients were included, reported a mortality of 17% and
18% in patients recipients of autologous (ASCT) and allogeneic stem cell transplantation (allo-SCT) respectively, compared with
a 31% mortality in non-SCT patients, prognostic factors for 45 day
overall mortality were age > 70 years, uncontrolled hematological
malignancy, ECOG 3–4, neutropenia (< 0.5 × 109/L) and a C-reactive
protein (CRP) > 20 mg/dL [9]. The EPICOVIDEHA, (Epidemiology
of COVID-19 Infection in Patients with Hematological Malignancies:
A European Hematology Association Survey), multinational project
included 3801 cases, represented by lymphoproliferative (mainly non-
Hodgkin lymphoma n = 1084, myeloma n = 684 and chronic lymphoid
leukemia n = 474) and myeloproliferative malignancies (mainly acute
myeloid leukemia n = 497 and myelodysplastic syndromes n = 279)
with an overall mortality of 31.2%, and the highest mortality observed
in acute myeloid leukemia (199/497, 40%) and myelodysplastic
syndromes (118/279, 42.3%); age, active malignancy, chronic cardiac
disease, liver disease, renal impairment, smoking history, and ICU
stay correlated with mortality [2]. A meta-analysis that included 3377
patients from Asia, Europe, and North America, found a 34% risk of
death for adult patients with hematologic malignancy and COVID-19,
whereas pediatric patients had a 4% risk of death [10]. A multicenter
study that included patients from Mexico, Peru, Guatemala and
Panama, reported a mortality of 37.7% in patients with COVID19
and hematological neoplasms, being higher in patients with acute
myeloid leukemia [11].
Another study conducted in the Mexican population, which
included four hundred thirty‐three patients with solid tumors (79%),
hematological neoplasms (21%) and COVID19 from the National
Cancer Institute of Mexico, reported one hundred thirty‐five (31%),
131 (30%), and 93 (21%) patients had obesity, hypertension, and
diabetes mellitus (DM), respectively and a mortality within 30 days
after diagnosis of 18% [12].
In our study we only included patients with hematological
neoplasms and COVID19 who were treated in hospital, therefore with
a more severe disease, which could explain the high mortality (50%),
patients with acute leukemia, mainly lymphoblastic leukemia (ALL)
were the most affected, and this is explained by the high population
that is treated in our institution with this disease. The prognostic
factors that we identified were age over 50 years and comorbidities
with a high prevalence in the Mexican population, such as diabetes
and hypertension, however, in the multivariate analysis, the CORADS
score ≥ 5 was the only factor associated with mortality which
can be related to COVID19 with well-defined radiological changes
and a more severe disease.
Conclusion
Different percentages of mortality and risk factors for patients
with COVID19 and hematologic malignancies have been reported,
depending on the geographical area and the characteristics of the
patients treated at their centers; however, it is common for the mortality of patients with hematological neoplasms to be increased.
In Mexico, factors such as the heterogeneity of hospital services, as
well as the comorbidities of the population can influence mortality.
Thanks to vaccination and prevention programs, COVID19 seems
to have decreased in our country, however, in other regions of the
world the activity of the disease is intense, so it is important to report
previous experience and take it as a basis to improve strategies for
patient care, especially those who are immunosuppressed, such as
patients with hematological malignancies.
References
Citation
Gilberto BL, Yubelka BM, Carlos MM, Humberto CS, Christian RP, et al. Survival of Patients with Hematologic Malignancies and
Covid-19. J Hematol Thromb 2022;7(1): 3.