Journal of Clinical and Investigative Dermatology
Download PDF
Case Report
Nursing-Specific Management on Toxic Epidermal Necrolysis (Ten) In Cml Patient: Case Report
Aswathy Asokan AN1*, Sachin SJ2, Chaitra P3, Jemy AM1, Aradhana KM1, Manjula MB1, Roselet J1, Goutham KJ1, Lakshmi A1 and Saranya UB1
1Department of Nursing, Hematology & Stem cell transplant, HCG Cancer
Hospital, Bangalore, India
2Head, Hematology & Stem cell transplant, HCG Cancer Hospital,
Bangalore, India
3Department of Dermatology, Hematology & Stem cell transplant, HCG
Cancer Hospital, Bangalore, India
4Department of Clinical Pharmacology, Hematology & Stem cell transplant,
HCG Cancer Hospital, Bangalore, India
*Address for Correspondence:
Aswathy Asokan AN, Department of Nursing, Hematology & Stem
cell transplant, HCG Cancer Hospital, Bangalore, India; Phone: +91
9590047671 E-mail: aswathy.a@hcgel.com
Submission: 28 Febraury, 2022
Accepted: 05 April, 2022
Published:09 April, 2022
Copyright: © 2022 Aswathy Asokan AN, et al. This is an open
access article distributed under the Creative Commons Attribution
License, which permits unrestricted use, distribution,
and reproduction in any medium, provided the original work is
properly cited.
Abstract
Toxic epidermal necrolysis (TEN) is a rare, life threatening, severe
mucocutaneous adverse reaction characterised by extensive
epidermal detachment, erosion of mucosae and severe constitutional
symptoms [1]. Worldwide, the incidence of TEN is estimated to be
between 1-2 per million people per year and in India 0.4 to 1.2 cases
per million people per year [2-5]. The mortality rate of TEN is about 20
to 60 percent [6,7]. Severe sepsis is an important complication and
main cause of death in TEN. The prognosis is improved by supportive
care especially with specialist nurses to achieve favourable outcomes
for patients [8].
Nursing care in TEN is paramount, as management focuses on
wound healing, infection prevention, hydration, nutrition, psychological
support and the prevention of long-term complications. Nurses, skilled
in infection prevention and barrier nursing are in an ideal position to
manage patients with TEN to achieve good outcome despite their
challenging disease course [9].
Case Presentation
A 53-year-old Indian woman who was on cancer chemotherapy
for chronic myeloid leukemia (CML) was admitted to our hospital
with a history of sudden onset itchy skin rashes on the body along
with fever chills. She had received Allopurionol, Hydroxyurea
and Dasatinib in the past 3-4weeks. Skin was erythematous, fragile
and more than 50% body surface area was involved. Mucosal
involvement was not present. Dermatologist opinion was sought and
was suspected to have cutaneous adverse drug reaction and all her
ongoing medications were temporarily withheld till recovery. She
was managed conservatively under the guidance of a hematologist,
dermatologist and infectious disease specialist. Treatment consisted
of IV fluids, systemic corticosteroids, antibiotics, antihistamines.
Patient recovered completely in 2 weeks of hospitalization and
was discharged. Her chemotherapy was resumed with alternative
medication Imatinib. She once again developed itching and rashes
within 2 weeks of starting medication, however, mild-moderate
in severity. Her symptoms were managed at home with oral
corticosteroids along with ongoing chemotherapy. The rashes
continued to progress in severity in spite of corticosteroids and
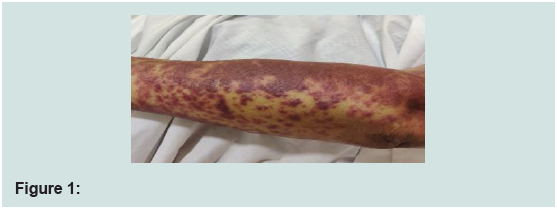
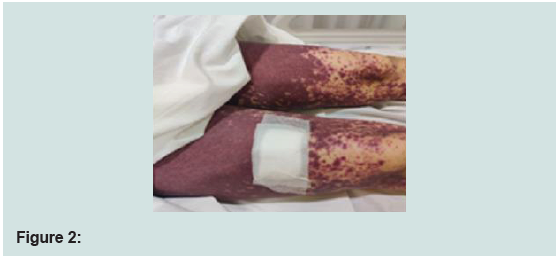
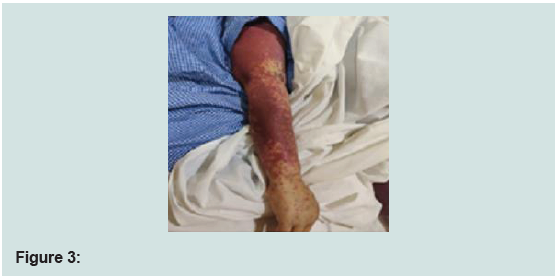
hence Imatinib was stopped. She developed blisters and exfoliation
of skin and was diagnosed to have toxic epidermal necrolysis (TEN)
involving 70-80% body surface area and oral mucosal erosions. She
was hospitalized and managed under close supervision by specialist
doctors and skilled nurses (Figures 1-3). She was treated with IV
fluids, corticosteroids, cyclosporine, antibiotics, antihistamines, daily
dressings with normal saline, liquid paraffin and mupirocin, oral care,
eye care, cannula care, high protein diet and strict infection control
measures. Vital parameters, blood counts and microbial cultures were
assessed closely and regularly. Patient’s condition improved and skin lesions were completely healed in about 3 weeks without scarring.
No complications in the form of secondary infections or systemic
morbidities were observed during her hospital stay.
In this case, the commonest nursing care interventions were
aggressive skin care, mucosal and eye care, infection surveillance
and prevention practices and general patient monitoring for
complications. Skin and wound care were most challenging part
of nursing care due to severe erosion or exfoliation. Nurses do not
use any specific guidelines of care but consider their role as a key in
quality outcomes for this patient.
Discussion
Patients with TEN presents with nuanced symptoms and have
complex nursing care needs. In the management of patients with
TEN, admission to a specialized burn centre or intensive care
setting may be considered. However, in our setting, this patient is
managed in haematology ward by nurses who are highly skilled in
barrier nursing and infection prevention with the guidance of expert
haematologists, dermatologist and infectious disease specialist. The
major nursing role in TEN is supportive, revolving around skin and
wound care, infection prevention, comfort management, hydration
and nutrition, psychosocial support, and the prevention of long-term
complications [10-12].
3.1. Focused nursing interventions executed for the patient:
A. Continuous Monitoring: Vital signs monitoring is an
essential part of management as they show the first sign of a
worsening systemic condition. We had monitored the parameters
such as body temperature, pulse rate, blood pressure, respiratory rate
and saturation rate every second hourly for the patient. Maintaining
Intake output chart is also equally important in patient with TEN in
order to prevent complications that arise from excessive fluid loss.
Intake- Output charting was done for the patient every 6th hourly.
We had examined mouth, eyes and genitalia (including perianal skin)
looking for mucositis, blisters and erosions during each nursing shift
as she was prone to infection. We had assessed patency of airway
and examined respiratory system to exclude pneumonia/respiratory
compromise.B. Maintenance of ambient room temperature: Keeping
the patient warm is a key nursing issue for the patients with TEN.
Patients was nursed in a room with environmental temperature
maintained at 30-32 degree Celsius which was ensured by keeping
the air conditioning was switched off and was provided with adequate
linen to ensure warmth. This has reduced caloric losses through the
skin and the resultant shivering and stress. Heat loss has also limited
by use of air-bed which had improved the comfort of the patient.
C. Pain and comfort: Pain management can be one of the most
challenging aspects of caring for patient with TEN. We had assessed
the pain levels using Wong-Baker Faces Rating Scale throughout
her hospitalisation and administered analgesics as per physician’s
order. We had always performed our nursing tasks like skin care,
bed changes during the peak effect of analgesics which had optimized
her comfort and compliance in care. Patient room has provided with
music, television and had permitted to keep idols of their favourite
God near the bed side so as to reduce the stress and provide comfort.
All efforts were made to provide the patient with the most comfortable
environment possible.
D. Nutritional considerations and fluid management: As
part of specific care, feeding and nutritional management is one
of the themes in nursing roles in the care of TEN patients. We had
ensured patient was on high protein diet and also included D protein
powder 1 tea spoon in milk for three times daily. We had provided
neutropenic soft, bland, nonacidic food for the patients since patient
had mild mucositis. The patient was on continuous IV fluids, Inj.
Normal saline@125ml/hr and strict I/O charting was maintained
every 6th hourly.
F. Oral care and ophthalmic surveillance: Oral hygiene had
maintained with chlorhexidine mouth wash (1:1 dilution with
drinking water) for gargling three times a day after food. We had
ensured patient used extra soft nylon bristled toothbrush and did
gentle brushing. Saline compression followed with paraffin ointment
every 2 hours was done on lips to soften the lips crusts and reduce the
pain. Daily assessment of mouth and surrounding areas was done.
Encouraged oral intake of the patient with soft, bland nonacidic food
which was micro waved. Ophthalmological consultation has taken
into priority place as soon as possible to determine the frequency of
surveillance. Symptomatic treatment aims to protect the cornea and
to maintain hydration of the eye surface, to minimize subsequent
problems; Supportive care is the mainstay of therapy. Local care had
administered by the instillation of an eye lubricant named Optive eye
drops, every 2nd hourly daily, helped in preventing irritation to the
eyes.
G. Infection prevention: Infection prevention is very crucial in
the management of these patients. Patient was admitted in a single
room equipped with dedicated equipment such as thermometer,
sphygmomanometer, pulse oximetry, cardiac monitor, and infusion
pumps. Availability of Alcohol hand rub outside the room was
ensured by the allocated staff nurse. Thorough environmental
cleaning, particularly the removal of dust from horizontal surfaces
was ensured on a daily basis. We had restricted the number of visitors
and made diligent hand washing, screening for illness and masking as
mandatory for visitors. Followed barrier nursing and sterile handling
of patients, Ensured that the allocated staff nurse is infection-free.
Regular hand hygiene with chlorhexidine hand rubs and hand
washes were practiced by health-care workers and caregivers. Always
use sterile gloves during aseptic or invasive procedures or contact with sterile sites. Monitored for foci of sepsis in the body through
daily assessment. We had avoided unnecessary insertion of urinary
catheters and Ryle’s tube. We had punctured and drained the skin
blisters rather than deroofing blisters. Peripheral venous cannulas
were handled minimally and left in place for a long duration and
not replaced before 96 h unless there was evidence of phlebitis,
local infection or malfunction. Activated sepsis protocols within 30
minutes of febrile episodes. Adhered strictly to neutropenic diet.
We had limited the patient movement and made arrangements for
portable diagnostic tests at bed side.
H. Psychological considerations: Providing emotional support
is a vital part of supportive care. We had used Distress Thermometer
scoring for this patient daily to assess her issues such as sleeping
difficulty, anxiety, maintaining relationships and being physically
intimate with her partner etc during hospital stay and addressed
these issues to the psycho-oncologist and had arranged regular follow
ups. Maintained good rapport with the patient and family and always
made available to them.
I. Informing the patient and the family: On discharge from
hospital, patient had received personalized information about the
suspected or proven cause of the disease, the risk of sequelae, the need
for follow-up and the possibilities for subsequent drug treatment. She
was instructed to avoid long time sun exposure which may worsen
pigmentation disturbances for several months or years and advised to
continue liquid paraffin to protect the skin Figure 1-3.
Conclusion
Toxic Epidermal Necrolysis (TEN) is most often the result of
an adverse drug reaction whose manifestation affect the skin and
mucous membranes and outcomes may be life threatening and fatal.
Supportive management has been proven to be the mainstay with
well executed nursing care resulting in quality clinical outcomes.
Supportive care is initiated earlier in the disease; mortality in TEN
will continue to decrease. Nurses are in a good position to help
patients avoid the long-term complications of this disease, promote
comfort, and improve survival by following these recommendations
for barrier nursing, daily care, surveillance, preventing infectioens
and the promotion of wound healing and recovery.
References
Citation
Aswathy Asokan AN, Sachin SJ, Chaitra P, Jemy AM, Aradhana KM, et al. Nursing-Specific Management on Toxic Epidermal Necrolysis (Ten) In Cml
Patient: Case Report. J Clin Investigat Dermatol. 2022;10(1): 3