Journal of Geriatrics and Palliative Care
Download PDF
Research Article
*Address for Correspondence: Nancy A Hodgson, Johns Hopkins University, School of Nursing, 525 Wolfe Street, Suite, 422 Baltimore, MD, 21205; voice 443-287-4503; E-mail: nhodgso1@son.jhmi.edu
Citation: Hodgson NA, Black BS, Johnston D, Lyketsos C, Samus QM. Comparison of Unmet Care Needs across The Dementia Trajectory: Findings from The Maximizing Independence at Home Study. J Geriatrics Palliative Care 2014;2(2): 5.
Copyright © 2014 Hodgson et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use,distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Geriatrics and Palliative Care | ISSN: 2373-1133 | Volume: 2, Issue: 2
Submission: 16 July 2014 | Accepted: 06 October 2014 | Published: 10 October 2014
Reviewed & Approved by: Dr. Rehan Aziz, Clinical Assistant Professor of Psychiatry at the Yale University School of Medicine and an Assistant Professor of Psychiatry at the University of Connecticut School of Medicine, USA.
Comparison of Unmet Care Needs across The Dementia Trajectory: Findings from The Maximizing Independence at Home Study
Nancy A Hodgson1*, Betty S Black2, Deirdre Johnston2, Constantine Lyketsos2 and Quincy M Samus2
- 1Center for Innovative Care in Aging, Johns Hopkins University, School of Nursing, USA
- 2Department of Psychiatry and Behavioral Sciences, School of Medicine, Johns Hopkins University, USA
*Address for Correspondence: Nancy A Hodgson, Johns Hopkins University, School of Nursing, 525 Wolfe Street, Suite, 422 Baltimore, MD, 21205; voice 443-287-4503; E-mail: nhodgso1@son.jhmi.edu
Citation: Hodgson NA, Black BS, Johnston D, Lyketsos C, Samus QM. Comparison of Unmet Care Needs across The Dementia Trajectory: Findings from The Maximizing Independence at Home Study. J Geriatrics Palliative Care 2014;2(2): 5.
Copyright © 2014 Hodgson et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use,distribution, and reproduction in any medium, provided the original work is properly cited.
Journal of Geriatrics and Palliative Care | ISSN: 2373-1133 | Volume: 2, Issue: 2
Submission: 16 July 2014 | Accepted: 06 October 2014 | Published: 10 October 2014
Reviewed & Approved by: Dr. Rehan Aziz, Clinical Assistant Professor of Psychiatry at the Yale University School of Medicine and an Assistant Professor of Psychiatry at the University of Connecticut School of Medicine, USA.
Abstract
Introduction: The aging of the population will bring with it an increase in the number of individuals with dementia living in the community. This will result in a greater demand on family caregivers and the long term care system to deliver care that is consistent with patient needs across the dementia trajectory, and requires a thorough understanding of an individual’s care needs as they change over the disease course. This study compares the unmet care needs of community dwelling persons with dementia across the stages of the dementia.Methods: Cross sectional analyses were conducted using in-home assessment data collected from 254 community residing persons with dementia and their informal caregivers.
Results and Discussion: Most unmet needs for patients in the early stage of disease were in the domains of safety and basic education about disease processes. Patients with moderate stage disease had the highest level of unmet needs in the domains of supervised daytime activities and caregiver’s management of neuropsychiatric behaviors. Individuals with severe or end stage disease had the highest level of unmet needs in the domain of emotional distress and the caregiver’s need for caregiver emotional support and respite. Reasons for unmet needs may be a consequence of a lack of knowledge about the disease process and a lack of psychosocial support resources. At all levels were evolving needs for information on the changing disease course and the need for meaningful activities. These results provide a basic overview of unmet needs by disease stage from which to build palliative care interventions for persons with dementia living at home and their family caregivers.
Keywords
Dementia care; Unmet needs; Patient-centered care; Caregivers; Care giving; Community-based careIntroduction
As society ages, the number of persons with Alzheimer’s disease and related dementias will increase [1]. Alzheimer’s disease is a progressive and fatal neurodegenerative disease for which there is no cure [2]. Most persons with dementia (PWD) prefer to remain at home for as long as possible, placing great demands on family caregivers [3]. For most PWD there is at least one family caregiver (CG) who faces increasingly complex and challenging problems as the disease progresses [4].A palliative approach to care, that emphasizes quality of life, dignity and comfort, is advocated for PWD beginning at the time of diagnosis and well before the need for specialist care or hospice care at end of life in order to enhance quality of life (QOL) [5,6]. Nonetheless most PWD receive little or no palliative care until death is imminent [6,7]. As no cure is in sight, it is critical to identify the unmet care needs of PWD living with the disease “upstream” in order to develop targeted palliative interventions. Introducing elements of palliative care earlier in the course of serious and incurable illness such as dementia is associated with enhanced quality of care [8].
Care giving and disease management needs for community dwelling PWD change as the disease progresses. Earlier studies on the unmet needs of PWD demonstrate a high level of care needs including personal care, household tasks, behavior problems and supervision. These studies have typically relied on CG’s perceptions of patient care needs with a focus on daily care giving tasks, have had only limited focus on CG’s own needs, and have not compared PWD and CG needs across stages of dementia [9,10]. Taking a multi-domain, clinician-rated approach to the assessment of PWD and CG needs, we recently reported that community-living PWD often had unmet home and personal safety needs, needs for meaningful activities and need for management of comorbid medical conditions, while common CG needs were for resource referrals and caregiver education [11]. Importantly, we found that higher unmet needs were not only associated with patient and caregiver socioeconomic status but with dementia stage.
This study aims to gain further insight into the specific types of unmet needs for community dwelling PWD and their caregivers across the stages of dementia using a comprehensive dementia care assessment approach. Specifically, we sought to 1) describe the unmet care needs across stages of dementia using a multidimensional needs assessment tool, and 2) compare the unmet needs identified across patients with mild, moderate or severe disease. A more precise understanding of basic unmet needs across the dementia trajectory can serve as an important platform on which to build and evaluate practical palliative care interventions for persons with dementia living at home and their family caregivers, and guide health care and long term care service redesign at both the federal and state level, as is the focus of the National Alzheimer’s Project Act (NAPA) and Affordable Care Act [12].
Methods
Using a cross sectional design, the unmet needs of PWD and their caregivers were assessed using baseline data collected between 2008- 2010 and before participant randomization into a trial evaluating a dementia care coordination intervention (the Maximizing Independence (MIND) at Home study) [11]. A total of 254 dyads (patients/caregivers) were enrolled in the study from the greater Baltimore, Maryland region. Inclusion criteria for the PWD were limited to community-residing, English-speaking, aged 70 and older with a confirmed cognitive disorder (mild cognitive impairment or dementia) and living in a geographically defined area (i.e. 28 postal codes in Baltimore, MD). Recruitment methods included obtaining referrals from community service organizations, sending letters to clients of community aging services, and promotions at local community events and through news media. A confirmed diagnosis of dementia was determined after an in-home clinician (geriatric psychiatrist, clinical nurse specialist) eligibility assessment. Informal caregivers were self-identified as having primary care responsibilities; age 21 years or older; English speaking; in contact with the primary participant at least once a week; and someone who the participant regularly relied on for assistance. Only participants who had informal caregivers are included in the current analyses (n=254).The Johns Hopkins Medicine Institutional Review Board approved this research. Oral consent was obtained for telephone screening interviews, and written consent was obtained for all participants at the in-home assessment. For those who lacked consent capacity, proxy consent was obtained from their legally authorized representatives as defined according to the Maryland Health Care Decisions Act, and assent was obtained from the cognitively impaired individuals.
Measurements
Primary participant demographic and socioeconomic data included age, sex, race, education, living arrangement, and income. Dementia severity was based on Mini-Mental State Examination (MMSE) [13] scores of 25-20 for mild, 11 to 20 for moderate, and <11 for severe [14]. Symptom severity was measured using the Neuropsychiatric Inventory Questionnaire NPI-Q, developed from the original NPI [15] based on caregiver report, and assesses the frequency (0 = never – 4 = very frequently) and severity (0 = none – 3 = marked: a major source of behavioral abnormality) of 12 behavioral domains, including delusions, hallucinations, agitation, aggression, dysphoria, anxiety, elation/euphoria, apathy/indifference, disinhibition, irritability/lability, aberrant motor disturbance, sleep disorders, appetite and eating disorders, and aberrant vocalizations [16], (α = 0.77 and 0.78, respectively, for sample) . Quality of life was assessed using the Quality of Life in Alzheimer Disease scale (QOL-AD), a dementia-specific brief 13-item inventory [17]. QOL-AD items reflect multiple dimensions (physical, social, emotional, and functional well-being) with each rated as 1 = poor, 2 = fair, 3 = good, or 4 = excellent. A total score representing the sum of items ranging from 13 to 52 was derived separately for patients and caregivers (α = 0.89 and 0.82, respectively). Depressive symptoms were assessed by means of the Cornell Scale for Depression in Dementia (CSDD), a 19-item depression scale (α = 0.76 for sample) [18].
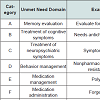
The Johns Hopkins Dementia Care Needs Assessment (JHDCNA) was used to identify participant and caregiver dementia-related needs [19]. A multidisciplinary group of clinical dementia care experts developed the JHDCNA, to identify 19 common dementia patients’ and caregivers’ needs and to document the extent to which those needs are met, based on established practices and guidelines [20-22]. The JHDCNA includes 15 care recipient need domains (A-O, 77 items) four caregiver need domains (Q-T, 12 items), and one “other/non specified” domain, with standardized descriptions and definitions for each item. The domains include safety, management of cognitive and non-cognitive symptoms, medical management daily activities, and a range of caregiver education and support needs (Table 1). Each domain contains multiple items that identify needs and each need is rated as unmet, or met. Clinicians completed the JHDCNA after each in-home assessment and based their judgments on interviews with the PWD and caregiver and a visual assessment of the PWD’s home and considered the individuals’ perspectives on their needs. A met need was defined as one that is being addressed and for which potential benefits of available interventions have been achieved to the extent possible for the individual. A need was considered unmet if it had not been addressed, and potentially beneficial interventions are available, or it had been or was being addressed, but potential benefits of available interventions had not been achieved.
Analyses
The data were analyzed to compare unmet needs by stage of illness using SPSS 19.0 (IBM Corporation, Armonk, NY), and P < .05 was considered statistically significant. Frequency distributions were determined to identify needs within the different domains. Crosstabs analysis were conducted to compare needs across disease stages using either chi square tests for categories with cells >5, or Fisher’s exact test for categories with cells <5.
Results
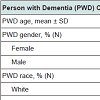
Table 2 describes the characteristics of the PWD and caregivers. The mean age of PWD was 83.6 ± 5.9; 167 (65.0%) were female, 172 (68.0%) were white, and 205 (81.0%) lived with others. Mean MMSE score was 17.7 ± 7.6, with 44.0% having mild, 38.0% moderate, and 18.0% severe dementia. The mean age of the caregivers was 66.1 ± 13.3. The majority of caregivers were female (75.0%), white (69.0%), non-spouses (59.0%), and not employed (51.0%). Caregivers reported that they spent an average of 6.7 ± 6.2 hours per day providing care to the PWD, and 22.0% rated their health as fair or poor.Table 3 presents the unmet needs that were found to be significantly different when compared across dementia stages. The leading unmet needs for individuals with early stage dementia were in the domains of Safety (I) and Caregiver Education (Q). PWD in the early stage had significantly more unmet needs for meaningful activities to prevent isolation (48.0% of total) when compared to PWD in the later stages of disease (p<.001). Early stage PWD also had significantly higher rates of need for evaluation regarding unsafe driving compared to other stages (90.6 % of total) (In addition, early stage PWD had significantly higher needs for medication assistance (p=.001) and supervision (p<.001) and treatment for cognitive and emotional symptoms with anticholinesterase medications (p=.010) (and antidepressants (.004) when compared to other stages.The leading unmet needs for individuals with moderate stage disease were in behavioral symptoms, most notably in wandering risk (52.3 % of total) and lack of supervision (53.3 % of total) when compared to the other stages. Caregivers of patients with moderate stage dementia also reported higher levels of need for respite when compared to other stages (p<.001). Among severe stage dementia patients, the highest unmet needs were in the safety domain item related to level of care. Caregivers of advanced stage dementia patients also reported higher unmet needs in the caregiver domain item related to emotional support Caregivers of patients with severe dementia also had higher rates of psychiatric symptoms (anxiety/depression) when compared to caregivers of earlier stage patients. Caregivers of advanced stage patients also reported higher levels of unmet needs regarding psychotropic medications not working and the need for anxiety management (p=.017) when compared to caregivers of patients with earlier stage dementia.
Discussion
Palliative care is appropriate at any stage of the dementia process. Earlier implementation of the palliative care approach is necessary if the needs of patients across the disease trajectory are to be adequately addressed. There is growing recognition among clinicians, researchers, and policy makers of the need for high-quality palliative care for patients with dementia, and that PWD have many unmet needs for palliative care [23,24]. Family caregivers will meet some of these needs, while professional palliative care providers will be needed to meet others. In order to promote comfort and quality of life in PWD across the disease trajectory palliative care, practitioners should take into account the changing care needs described here.The PWD in this study had many needs across the trajectory of the disease, varying from memory support and the need for attention to safety in early stage to the need for emotional support for both patients and caregivers in severe stage dementia. Regardless of dementia stage, there remains a high level of unmet needs for education about the disease process management of behavioral symptoms and the emotional needs of caregivers. Despite the availability of these services in many communities, one explanation that these needs remain unmet is that PWD and CG were not aware of the service offerings available or there were mismatches between the way in which services are offered and the individual needs of PWD and CG [25].
Palliative care professionals should be aware of the upstream needs for clear, up-to-date, information on topics such as driving safety and medication management to slow the course of cognitive decline in early stage patients. This is particularly relevant given the current trends toward earlier recognition and the development and application of biomarkers. For individuals with moderate stage disease, the study revealed a substantial need for palliative interventions to help CG address the unmet needs for neuropsychiatric symptoms. Finally, sensitive discussion of the emotional needs of CG and the emergence of anxiety symptoms is an essential component of care for individuals in the severe stage.
Some caution is required for the interpretation of the results. The needs assessment tool was primarily designed to assess needs of PWD and CGs from a clinician perspective, not primarily based on the patient or family’s perspectives on their own needs. While the clinician rating of each unmet need calls for taking into account the perceptions of the family desires, needs, and preferences, the rating did not include formal input from family on the weight or importance of each need. Moreover the instrument was not tailored to examine stage-specific needs and therefore may not have captured some specific and important stage-specific needs. The results of the study are not generalizable to PWD residing in institutional settings. Participants were not randomly selected and were recruited from one urban geographic area, further limiting generalizability. Another limitation is missing data. It is possible that data were not missing at random. For example, individuals with low income may be less likely to answer questions about income, and that those in the severely demented group were less likely to complete questionnaires on depression and quality of life than early and moderate stage participants.
The aim of palliative care is to address unmet needs that contribute pain and suffering and to support the patient and family in achieving the best quality of life possible. This definition of care is highly consistent with health care reform goals in that palliative care is multidisciplinary, coordinated across multiple settings, and inherently person-, and family-centered. Given the central role of family caregivers for persons with dementia, it is essential to bring family caregivers into the discussion, hear their concerns, and develop meaningful responses to address their unmet needs.
Palliative dementia care requires a specialized knowledge base since the trajectory and symptoms differ in important ways from other conditions [26]. Knowledgeable caregivers are needed to ensure a safe and supportive environment where the individual’s dignity is protected and quality of life is maximized. Longitudinal research is needed to examine the changing needs over time and to identify the evolving information needs of caregivers. These findings can contribute to the development of practice guidelines for this specific patient population in palliative care.
For individuals with dementia to live safely and comfortably in the community for as long as possible, it is imperative that their needs for care, services, and support; and those of their CG are met. The unmet needs identified included the need for increasing assistance with instrumental and basic activities of daily living (ADLs), meaningful activities suited to their interests and capabilities, treatment and management of dementia-related symptoms, and care for coexisting physical illnesses. As palliative care moves “upstream,” earlier in the course of dementia, and into the mainstream of dementia practice, knowledge of these evolving unmet needs across the disease trajectory can be used to inform a comprehensive palliative approach from the point of diagnosis through the end of life.
References
- Rocca WA, Petersen RC, Knopman DS, Hebert LE, Evans DA, et al. (2011) Trends in the incidence and prevalence of Alzheimer’s disease, dementia, and cognitive impairment in the United States. Alzheimers Dement 7: 80-93.
- Hughes JC, Jolley D, Jordan A, Sampson EL (2007) Palliative care in dementia: issues and evidence. Adv Psychiatr Treat 13: 251-260.
- Brodaty H, Donkin M (2009) Family caregivers of people with dementia. Dialogues in Clinical Neuroscience: 217-228.
- Messinger-Rapport B, McCallum TJ, Hujer ME (2006) Impact of Dementia Caregiving in the Caregiver in the Continuum of Care. The annals of long-term care 14: 34.
- Volicer L (2006) Goals of care in advanced dementia: quality of life, dignity and comfort. The Journal of Nutrition, Health & Aging 11: 481.
- Sampson EL, Ritchie CW, Lai R, Raven PW and Blanchard MR, et al. (2005) A systematic review of the scientific evidence for the efficacy of a palliative care approach in advanced dementia. International Psychogeriatrics 17: 31-40.
- Mitchell SL, Teno JM, Kiely DK, Shaffer ML, Jones RN, et al. (2009). The clinical course of advanced dementia. N Engl J Med 361: 1529-1538.
- Diwan S, Hougham GW, Sachs G (2004) Strain experienced by caregivers of dementia patients receiving palliative care: findings from the Palliative Excellence in Alzheimer Care Efforts (PEACE) Program. Journal of Palliative Medicine 7: 797-807.
- Gaugler JE, Kane RL, Kane RA, Newcomer R (2005) Unmet care needs and key outcomes in dementia. Journal of the American Geriatrics Society 53: 2098-2105.
- Geraldine A Hancock, Bob Woods, David Challis and Martin Orrell (2006) The needs of older people with dementia in residential care. International Journal of Geriatric Psychiatry 21: 43-49.
- Betty S Black, Deirdre Johnston MB, Peter V Rabins, Ann Morrison, Constantine Lyketsos, et al. (2013) Unmet Needs of Community-Residing Persons with Dementia and Their Informal Caregivers: Findings from the Maximizing Independence at Home Study. Journal of the American Geriatrics Society 61: 2087-2095.
- US Department of Health and Human Services. National Alzheimer's Project Act (NAPA).
- Folstein MF, Folstein SE, McHugh PR (1975) Mini-Mental State: A practical method for grading the cognitive state for patients for the clinician. J Psychiatr Res 12: 189-198.
- Perneczky R, Wagenpfeil S, Komossa K, Grimmer T, Diehl J, et al. (2006) Mapping scores onto stages: mini-mental state examination and clinical dementia rating. Am J Geriatri Psychiatry 14: 139-144.
- Cummings JL, Mega M, Gray K, Rosenberg-Thompson S, Carusi DA (1994) The Neuropsychiatric Inventory: comprehensive assessment of psychopathology in dementia. Neurology 44: 2308-2314.
- de Medeiros K, Robert P, Gauthier S, Stella F, Politis A, et al. (2010) The Neuropsychiatric Inventory-Clinician rating scale (NPI-C): reliability and validity of a revised assessment of neuropsychiatric symptoms in dementia. Int Psychogeriatr 22: 984-994.
- Logsdon RG, Gibbons LE, McCurry SM, Teri L (2002) Assessing quality of life in older adults with cognitive impairment. Psychosom Med 64: 510-519.
- Alexopoulos GS, Abrams RC, Young RC, Shamoian CA (1988) Cornell Scale for Depression in Dementia. Biol Psychiatry 23: 271-284.
- Johnston D, Samus QM, Morrison A, Leoutsakos JS, Hicks K, et al. (2011) Identification of community-residing individuals with dementia and their unmet needs for care. Int J Geriatr Psychiatry 26: 292-298.
- Callahan CM, Boustani MA, Unverzagt FW, Austrom MG, Damush TM (2006) Effectiveness of Collaborative Care for Older Adults with Alzheimer Disease in Primary Care: a randomized controlled trial. JAMA 295: 2148-2157.
- Rabins PV, Lyketsos CG, Steele CD (2006) Practical Dementia Care, 2nd Edition. New York: Oxford University Press.
- Lyketsos CG, Colenda CC, Beck C, Blank K, Doraiswamy MP, et al. (2006) Position Statement of the American Association for Geriatric PsychiatryRegarding Principles of Care for Patients With Dementia Resulting From Alzheimer Disease. Am J Geriatr Psychiatry 14: 561-572.
- Miranda-Castillo C, Woods B, Orrell M (2013) The needs of people with dementia living at home from user, caregiver and professional perspectives: a cross-sectional survey. BMC Health Serv Res 13: 43.
- Van der Roest HG, Meiland FJ, Maroccini R, Comijs HC, Jonker C, et al. (2007) Subjective needs of people with dementia: a review of the literature. Int Psychogeriatr 19: 559-592.
- Brodaty H, Thomson C, Thompson C, Fine M (2005) Why caregivers of people with dementia and memory loss do not use services. Int J Geriatr Psychiatry 20: 537-546.
- van der Steen JT, Radbruch L, Hertogh CM, de Boer ME, Hughes JC, et al. (EAPC) (2014). White paper defining optimal palliative care in older people with dementia: A Delphi study and recommendations from the European Association for Palliative Care. Palliat Med 28: 197-209.